Research Article
Effect of Educational Plan on Adherence Rate among Children with Persistent Asthma
Tuberculosis and Lung Diseases Research Centre, Tabriz University of Medical Sciences, Tabriz, Islamic Republic of Iran
Asthma management has improved markedly over the last 50 years, largely due to the introduction of inhaled corticosteroids (ICS) in the early 1980s. These agents are now considered to be the cornerstone of therapy for persistent asthma of all degrees of severity in adults and children. Nevertheless, good-quality outcome in asthma hinge not just on the availability of medication but also on their appropriate use by patients (Horne, 2006).
Adherence to medication can be defined as the degree to which use of medication by the patient correspounds with prescribed regimen. Different studies indicate that primary non adherence (not filling initial prescription) ranges from 6-44% and secondary non adherence (rate of medication use) is often poor (World Health Organization, 2003).
One study examined the relationship between the asthma management strategies used by 101 parents of children with asthma and the perception of these parents of their child`s vulnerability to illness. The study found that after controlling for frequency and severity of asthma symptoms, those parents who felt their child had greater vulnerability to illness, were more likely to use regular preventive medications, take the child to doctor and keep him or her home from school. The authors suggested that one possible explanation of this finding is that parents who do not perceive their child to be medically vulnerable may discontinue administering regular medication (Spurrier et al., 2000).
However medication adherence is a complex issue involving the child, family members and other care givers (Gradiner and Duorkin, 2006).
This process depends on family cultural beliefs, their perception of disease severity and understanding of the benefits of treatment.
The study by Horne (2006) showed that patients were significantly more likely to endorse the personal need for regular ICS if they shared the medical view of asthma as an acute on chronic condition, it means that asthma is a chronic disease that manifest as acute symptomatic flare-up or attack.
In contrast, other patient`s models of asthma were more closely linked to symptom experience. These patients considered themselves to be well when asthma symptoms were absent and took ICS sporadically in response to symptoms (Horne and Weinmon, 2002).
Based on Cochran study which was conducted as systematic review, over all, patients took the recommended doses of medication on 20-73% of days. The percent of underused days ranged from 24-69% and the overuse 2-23%. Average compliance, measured as a ratio of doses taken to doses prescribed, ranged from 63-92% (Cochrane et al., 2000).
Therefore the outcome of non adherence is loss, loss of opportunities for patients to improve their health and loss of medication by health-care systems, with subsequent effect of increased mortality. All of these are greatly concerning given the vulnerability of these patients to progressive, irreversible airway obstruction (Horne, 2006).
In fact, the adherence is key mediator between medical activities and outcome of disease.
All above mentioned issues indicate that asthma is a complex disease which needs family and patient`s education and refer to the following key points: (a) patient education, beginning at the time of diagnosis and integrated into every steps of asthma care; (b) patient education provided by all members of team; (c) teaching asthma self-management skills by tailoring information and a treatment approach to fit the needs of each patient; (d) teaching and reinforcing behavioral skills such as inhaler use, self monitoring and environmental control; (e) joint development of treatment plans by team members and patient; (f) encouraging adherence to the treatment plan jointly developed by the interdisciplinary team and patients. Therefore this study was conducted to survey the effect of education and regular follow up visits on adherence rate among children with mild to moderate persistent asthma.
In a semi-experimental study (before and after), two groups of children with mild to moderate persistent asthma, referred to outpatient clinic of Tabriz University of Medical Sciences were compared.
First group included 200 asthmatic children who had been treated between Feb. 2004-Feb. 2006 at least for duration of one year by conventional method.
The second group included 300 patients at the same age and severity of disease that were treated between Feb. 2006-Feb. 2008 at least one year by a comprehensive plan of education and regular follow up visits as well.
Patients who were at the same age and had mild to moderate persistent asthma were included in study and patients with intermittent or sever persistent asthma were excluded. The disease of the patients was physician diagnosed and they were treated by ICS via spacer. Severity of asthma was assessed by Global Initiative for Asthma (GINA) guideline. Data were extracted from patient`s files. Parents gave informed consent and background information used to classification was obtained from parental reports.
| Table 1: | Patient characteristics in two groups |
 | |
In this study good adherence and poor adherence were defined as ≥50% and <50% respectively and estimated adherence was operationalized as the ratio of the number of puffs used over the study period to the number of puffs prescribed by Celano et al. (1998).
Data were analyzed by statistical software spss13 and Chi-square test. p-value ≤0.05 was defined as significant. Background characteristics of the study sample are presented in Table 1.
Findings indicate that in first group 100 patients (50%) and in second group 295 patients (84/3%) had adherence rate of more than 50% (p = 0.00), as is presented in Table 2.
Based on the findings on Table 3 and considering adherence rate of ≥50%, there is significant difference between two groups in patients with mild persistent asthma (p = 0.00).
But regardless of percent differences in the patients with moderate persistent asthma, p-value is not significant (p = 0.1). However in first group, based on the disease severity (mild and moderate), difference of adherence rate is not significant (p = 0.7), in contrast second group shows significant difference (p = 0.00).
This study was conducted to assess the effect of education and scheduled follow up visits on adherence rate of ICS in children with mild to moderate persistent asthma. Based on findings, good adherence (≥50%) increased from 50% (before) to 84.3%. In a research on 61 children with 6-17 years old, only 34 patients continued the study. The findings indicate that adherence rate was 44% and just 12% of patients showed the rate of 75% (Celano et al., 1998).
In another study on 106 patients in age group of 3-16 years old, the asthmatic patients represented a wide range of adherence, from those who took none of their prescribed doses to those who took practically all (99%) of their prescribed doses. The mean level of adherence was 0.48, indicated that on average, children took approximately half of their prescribed medications. In this study the adherence rate did not differ by asthma severity (McQuaid et al., 2003). In contrast in our study and in the patients with mild persistent asthma there was significant difference between before and after intervention. But there was no difference in patients with moderate persistent asthma (p = 0.1).
| Table 2: | Adherence rate before and after intervention |
| p = 0.00, Values shown in parenthesis are in percentage | |
| Table 3: | Adherence rate based on disease severity |
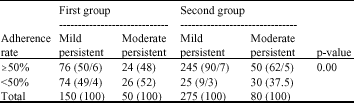 | |
| Values shown in parenthesis are in percentage | |
Meanwhile, when two groups were analyzed isolated, although there was no significant difference in first group (p = 0.1) but in contrast, in the second group, the adherence rate of patients with mild persistent was high as well (p = 0.00).
We think that complexity of treatment in moderate persistent asthma can explain these findings. One study showed that the cohort that used fluticasone plus salmetrol from a single inhaler had significantly better adherence than the other cohort that used these medications from separate inhalers (Stoloff et al., 2004).
However, another study showed that the patients who report they have severe asthma or believes that asthma is serious health problem are more likely to report regular use of preventive/anti-inflammatory medications for asthma (Chambers et al., 1999).
It is obvious that developing such perception of asthma needs suitable education and Gallefoss and Bakke (1999) believes that the patient education on asthma medications and self-management skills can improve adherence with inhaled steroids and management skills for acute exacerbations. And this study indicates that patient education about self-management could increase the adherence rate from 32 to 57%. Although this study has promoted adherence rate but is not comparable with this study. In a study researchers investigated the effect of four 90 min education sessions and written guidelines on adjusting inhaled medication plans. They found that mean compliance improved 83±38% in the run-in period to 92±52% after education, which is similar to present findings of van der Palen et al. (1997).
Inhaler corticosteroids are the cornerstone of asthma medication and adherence to these drugs is related to mortality and morbidity. Present findings indicate that education and scheduled follow up can result in higher degree of adherence.
This study was supported by a grant of Tuberculosis and Lung Research Center, Tabriz University of Medical Sciences (grant No. 86/10).