Research Article
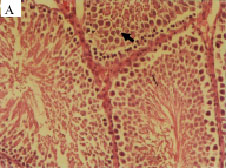
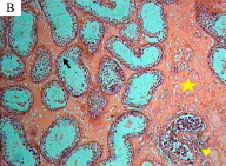
Comparative Study of the Effects of Gentamicin, Neomycin, Streptomycin and Ofloxacin Antibiotics on Sperm Parameters and Testis Apoptosis in Rats
Department of Veterinary Pathology, Islamic Azad University Tabriz Branch, Iran
Marefat Ghaffari Novin
Cellular and Molecular Biology Research Center, Shaheed Beheshti University MC, Tehran, Iran
Amir Afshin Khaki
National Management Center for Health (NPMC), Department of Anatomical Science,Tabriz University of Medicine Science, Tabriz, Iran
Mohammad Nouri
Department of Biochemistry Science, Tabriz University of Medicine Science, Tabriz, Iran
Ehsan Sanati
Department of Veterinary Pathology, Islamic Azad University Tabriz Branch, Iran
Mahdad Nikmanesh
Department of Veterinary Pathology, Islamic Azad University Tabriz Branch, Iran











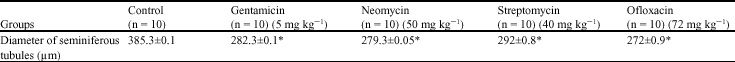

professor ehsan Reply
this is very good and scientific papers.
Ehsan m Reply
good researh paper