Research Article
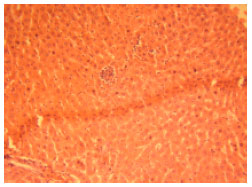
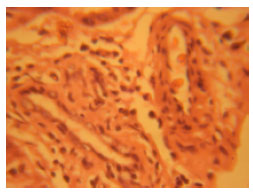
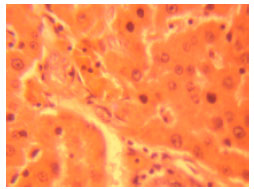
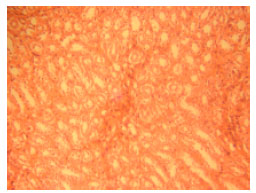
Phytochemical and Toxicological Studies of Aqueous Leaves Extracts of Erythrophleum africanum
Department of Biochemistry,
M. J. Ladan
Department of Biochemistry,
R. A. Dogondaji
Department of Biochemistry,
R. A. Umar
Department of Biochemistry,
L. S. Bilbis
Department of Biochemistry,
L. G. Hassan
Department of Pure and Applied Chemistry,
A. A. Ebbo
Department of Veterinary Physiology and Pharmacology, Usmanu Danfodiyo University, P.M.B. 2346, Sokoto, Nigeria
I. K. Matazu
Department of Biochemistry,