Research Article
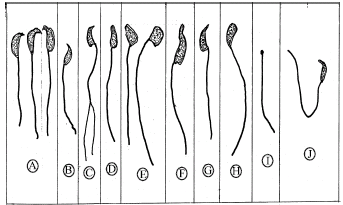
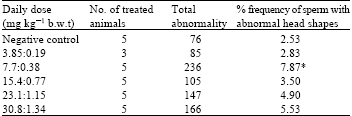
An in vivo Evaluation of the Induction of Abnormal Sperm Morphology by Sulphamethoxypyridazine: Pyrimethamine (Metakelfin®)
Department of Zoology, University of Lagos, Lagos, Nigeria
A.A. Mosuro
Department of Basic Sciences, Botswana College of Agriculture, Private Bag 0027, Gaborone, Botswana, Nigeria