Research Article
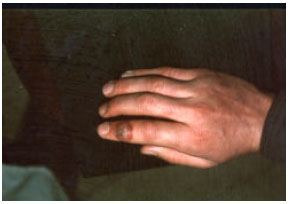
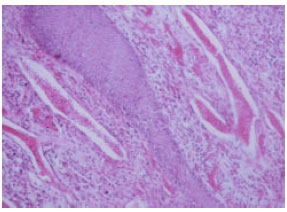
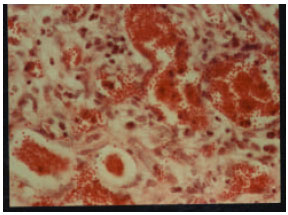
Contagious Ecthyma: Case Report and Review
Department of Pathology, School of Veterinary Medicine, Shahrekord University, Shahrekord, Iran
M. Maleki
Department of Pathology, School of Veterinary Medicine, Ferdowsi University, Mashhad, Iran