Research Article
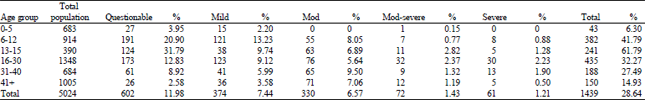
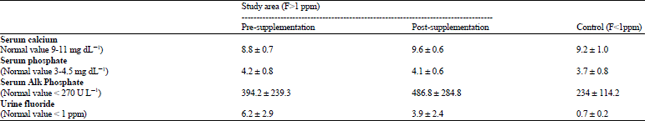
Prevalence of Dental Fluorosis and the Role of Calcium Supplementation in its Prevention
Department of Pathology and Microbiology, Saraswati Dental College, Lucknow, India
Aditi Singh
Amity Institute of Biotechnology, Amity University Uttar Pradesh, Lucknow Campus, Lucknow, India
LiveDNA: 91.17399
Parul Tripathi
Amity Institute of Biotechnology, Amity University Uttar Pradesh, Lucknow Campus, Lucknow, India
Asha Mathur
Department of Pathology and Microbiology, Saraswati Dental College, Lucknow, India