Research Article
Urinary Bladder Cancer: A Clinicopathological and Histological Study
Karpagam University Coimbatore, India
P. Chinnaswamy
Karpagam University Coimbatore, India
Urinary bladder cancer is the most common malignancy of the urinary tract, responsible for significant mortality and morbidity worldwide (Kirkali et al., 2005). It is seen mainly in men. The incidence in women is approximately 3-4 times lower than in men but it seems to be rising (Rafique and Javed, 2006). The American cancer society reported that about 69,250 new cases of urinary bladder cancer (52,020 men and 17,230 women) were diagnosed whereas, 14,990 cases died (10,670 men and 4320 women) in 2011. Although, bladder cancer ranks lower in total number of cancer related deaths than it does in incidence, it has the eminence of being the malignancy with the fastest rate of recurrence which results in a very high prevalence (Srivastava et al., 2013). The incidence increases with age (median age 69-70 years), smoking, living in urban areas and working in dye, rubber or leather industries.
Nearly 80% of patients who initially present with bladder urothelial carcinoma have tumors confined to the mucosa or sub mucosa, so called superficial non-muscle invasive bladder cancers, more appropriately reported as stage Ta or T1 urothelial tumors. These tumors represent a heterogeneous group of lesions. The CIS have been included historically as part of the group of superficial bladder cancer. The remaining bladder tumor invading the muscular is propria of the bladder or beyond (Lopez-Beltran, 2008). To date, an adequate tool for screening urinary bladder cancer has not been established. Under these circumstances, the symptomatology of disease including haematuria, remains important both for clinicians and patients (Badar et al., 2009). Gross or microscopic painless haematuria is the most common presentation (Ahmed et al., 2002). It is estimated that approximately 20% of patients being evaluated for gross haematuria will subsequently be diagnosed with bladder cancer. The vast majority of bladder cancers are diagnosed as a result of evaluating patients for haematuria. Total gross haematuria without pain is the typical sign of suspicion for bladder cancer. Similarly, in patients presenting with microscopic haematuria, upto 10% will be diagnosed with bladder cancer. One-quarter patients with bladder cancer will present with irritative voiding symptoms of urgency, frequency and dysuria, symptoms frequently misinterpreted as urinary tract infection but that may signify either trigone involvement with tumor or the presence of CIS (Lopez-Beltran, 2008).
A reliable grading and staging system is needed to stratify the patients into prognostically distinct groups and allow for comparison of treatment results among institutions (Cheng et al., 2000). Urine cytology may be performed, however, diagnosis usually requires cytoscopy and biopsy. These two had been regarded as the gold standard in the diagnosis of bladder cancer and in the follow up of these patients (Kundra and Silverman, 2003). Transurethral resection of the bladder tumor (TURBT) is the initial and critical step in the management of non-muscle-invasive tumors. This procedure not only removes all visible lesions but also provides tumor specimens for pathological evaluation (Ukai et al., 2010). The main objective of the present study is based on TURBT results to establish the histologic diagnosis of the bladder tumor, determine the tumor stage (the pathologist must be able to evaluate the depth of tumor invasion from the surgical specimen), determine all clinically important prognostic factors such as the grade, number and size of the tumor.
MATERIAL AND METHODS
The study population consisted of 70 patients who underwent TURBT at Vedhanayagam hospital, Coimbatore. All patients underwent TURBT at a single institution. The biopsy report obtained by TURBT of the primary tumor of the all 70 patients were collected and pathological diagnosis was made according to the World Health Organization (WHO)/International Society of Urological Pathology (ISUP) classification in 2004 (Vaidya et al., 2013) and the tumors were graded as low and high grade urothelial Transitional Cell Carcinomas (TCC). According to the TNM (tumor, lymph node, metastasis) classification (Table 1) the data recorded as tumor limited to mucosa, invasion of lamina propria and invasion of muscle.
| Table 1: | Tumor Node Metastases (TNM) classification of bladder cancer (2002 revision) |
 | |
Seventy patients were taken for the study and the age group ranges from 52-87 years with a mean of 67.87 and the results were shown in the Fig. 1.
TCC cases were papillary, 9 (12.5%) were solid, the cells were identical to normal urothelium, absences of mitosis and the presence of single layer cuboidal cells whereas, 61 (87.5%) were both papillary and solid with ordered or disorders cells, crowding, frequent loss of polarity with moderate-marked pleiomorphism and variable thickness and the results were shown in Fig. 2.
Nine out of 70 patients (12.8%) showed tumor size of 4-5 cm, 18 patients out of 70 (25.7%) showed a tumor size of 3-3.5 cm and 35 out of 70 patients (50%) showed tumor size of 1-2.5 cm. TCCs showed histological signs of 18 out of 70 patients with muscle invasion (infiltrative) at diagnosis, 53 out of 70 patients without muscle invasion. The 61 out of 70 (87%) patients have shown the lamina propria invasion, 18 out of 70 (25.7%) have shown lymph vascular space invasion and results were shown in Fig. 3.
Among the 70 patients, 44/70 (63%) are of high grade and 17 out of 70 (24%) are of low grade and the results were shown in Fig. 4.
Urinary bladder neoplasms are heterogeneous group of tumors with different subtypes and behavioural patterns, therefore, the epidemiological and clinicopathological comparison is relatively very difficult (Gupta et al., 2009). Cystoscopy and biopsy are the main diagnostic measures and most of the specimens in our study were TURBT.
Bladder cancer is rare in people younger than 50 years of age, even though it can occur at any age. Incidence of cancer increases with age with median age at diagnosis around 70 years (Laishram et al., 2012). In our study, 87.5% patients were older than 60 years at the time of presentation which is similar to study inwhich 73.07% patients were older than 50 years (Laishram et al., 2012). Younger patients frequently present with lower grade and lower stage tumors than their elder counterparts (Wan and Grossman, 1989). Transitional Cell Carcinoma (TCC) was the most common bladder neoplasm in our study and was diagnosed in 61 (87.50%) cases. Similar data (81.81%) was published by Mahesh and Yelikar (2012) from India. Small cell carcinoma and adenocarcinoma are uncommon tumors of the bladder and account for about 0.5 and 2% of all bladder cancers, respectively (Vaidya et al., 2013) which coincides with our study, where 1 (8.75%) case of an adenocarcinoma was seen.
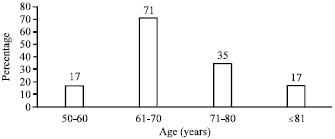 | |
| Fig. 1: | Relationship between age and incidence |
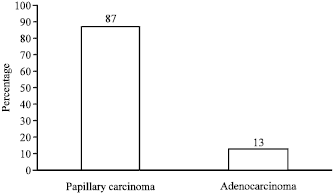 | |
| Fig. 2: | Relationship between papillary and adenocarcinoma |
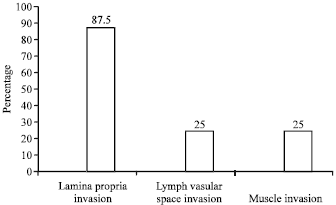 | |
| Fig. 3: | Relationship between muscle invasion, lamina propria invasion, lymph vascular space invasion |
Histologic grading of the tumors was done according to WHO in 2004/ISUP (Vaidya et al., 2013) grading of the urothelial neoplasm. In our study, high grade was 44 cases (62.85%) and low grade was in 18 cases (25%). This may be due to the patient’s late presentation. Vaidya et al. (2013) also observed higher incidence of high grade TCC (43.21%) cases and low grade as 39.51%. Pathologic grade and muscle invasion are the most valuable prognostic predictors of survival.
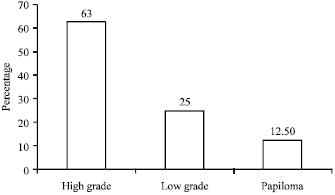 | |
| Fig. 4: | Relationship between the high grade and low grade tumors |
In our study, the muscle invasion was in 18 (25%) patients, the lamina propria invasion was in 61 (83%) and the lymph vascular invasion seen in 18 (25%) which is similar to the observations (18 and 75%, respectively) reported by Laishram et al. (2012).
In our study, bladder tumors were the commonest lesions seen in cystoscopic biopsies, most of which were of urothelial origin. Transitional cell carcinoma was the most common bladder tumor in our study. Most of these tumors were high grade. A large percentage of high grade transitional cell carcinomas presented with muscle invasion. Pathological grade and muscle invasion are the most valuable prognostic predictors of survival. The importance of including smooth muscle in the biopsy specimens needs to be emphasized and also awareness is needed among the public as they may tend to neglect the haematuria resulting in an advanced stage of bladder cancer at the time of presentation.