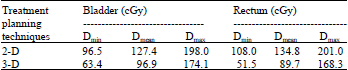Research Article
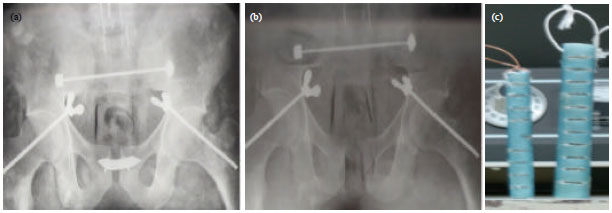
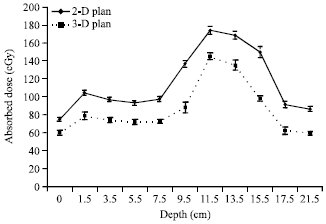
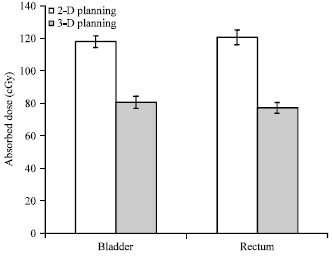
Comparison of Radiation Absorbed Dose Received by Bladder and Rectum between Conventional and Conformal Treatment Planning Methods in Radiotherapy of Prostate Cancer
Department of Medical Physics and Biomedical Engineering, Kermanshah University of Medical Sciences, Kermanshah, Iran
Seyed Ali Rahimi
Health Sciences Research Center, Mazandaran University of Medical Sciences, Kilometer 18 Khazarabad Road, Sari, Iran