Research Article
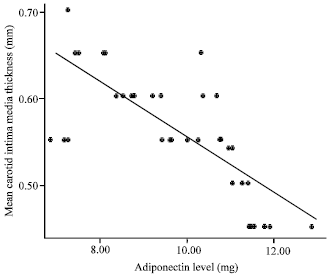
Normal Adiponectin Level and Glycemic Control could Delay Subclinical Atherosclerotic Changes in Lean Type 1 Diabetic Children
Department of Pediatrics,Faculty of Medicine, Suez Canal University, Egypt
Hassan Shora
Department of Medicine,Faculty of Medicine, Suez Canal University, Egypt
Hanaa Fahmy
Department of Clinical Pathology, Faculty of Medicine, Suez Canal University, Egypt