Research Article
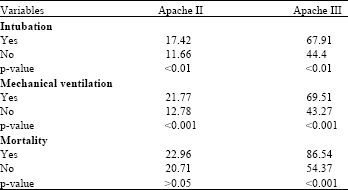
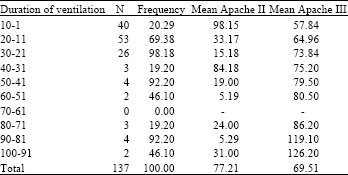
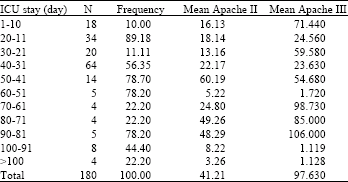
Analyzing the Efficacy of Apache III versus Apache II on Duration of Mechanical Ventilation and ICU Stay
Department of Neurosurgery, Kashani Hospital, Isfahan University of Medical Sciences, Isfahan, Iran
M. Masoudifar
Department of Anesthesiology, Kashani Hospital, Isfahan University of Medical Sciences, Isfahan, Iran
M. Sabouri
Department of Neurosurgery, Kashani Hospital, Isfahan University of Medical Sciences, Isfahan, Iran
F. Rouhani
Department of Anesthesiology, Kashani Hospital, Isfahan University of Medical Sciences, Isfahan, Iran
M. Arrabian
Department of Neurosurgery, Kashani Hospital, Isfahan University of Medical Sciences, Isfahan, Iran