Case Study
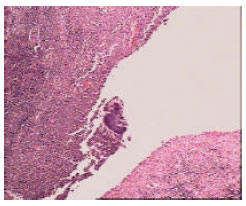
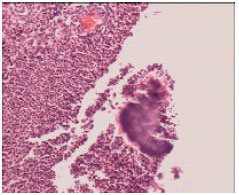
Meckel’s Diverticulitis Due to Actinomycosis
Department of General Surgey, Gorgan University of Medical Sciences, P.O. Box, 49175-553 Gorgan, Iran
Ramin Azarhoush
Department of Pathology, Gorgan University of Medical Sciences, Iran
Mohammad Jafar Golalipour
Department of Embryology and Histology, Gorgan University of Medical Sciences, Gordan, Iran