Research Article
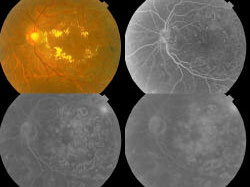
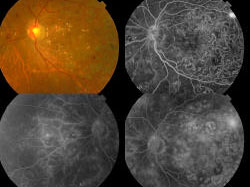
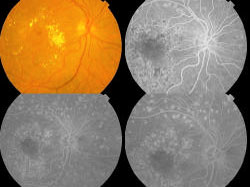
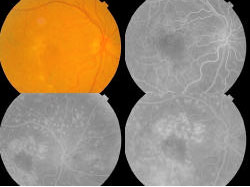
High Dietary Fibre Intake (Talbina) as Adjunct in the Management of Diabetic Macular Edema
Department of Ophthalmology, Al Azhar University, Egypt
Hayam S. Kamel
Department of Ophthalmology, Al Azhar University, Egypt
Mohamed A. El Malt
Research Institute of Ophthalmology, Cairo, Egypt