Research Article
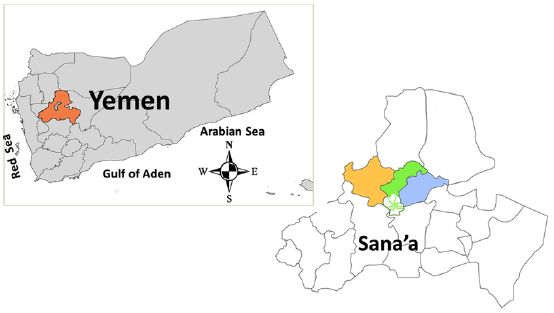
Nasal Carriage of Staphylococcus aureus Among Students of Public Schools in Sana’a, Yemen
Department of Medical Microbiology, Faculty of Medicine and Health Sciences, Sana`a University, Sana`a, Yemen
LiveDNA: 969.5313
Jawaher. M. Hauter
Department of Medical Microbiology, Faculty of Medicine and Health Sciences, Sana`a University, Sana`a, Yemen
Noria H. Al-Bulili
Department of Medical Microbiology, Faculty of Medicine and Health Sciences, Sana`a University, Sana`a, Yemen
Rasha A. Al-Hotami
Department of Medical Microbiology, Faculty of Medicine and Health Sciences, Sana`a University, Sana`a, Yemen
Maha T. Al-Horaibi
Department of Medical Microbiology, Faculty of Medicine and Health Sciences, Sana`a University, Sana`a, Yemen