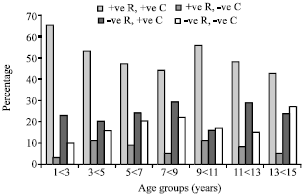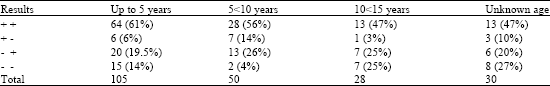Research Article
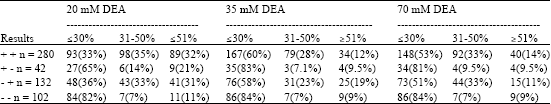
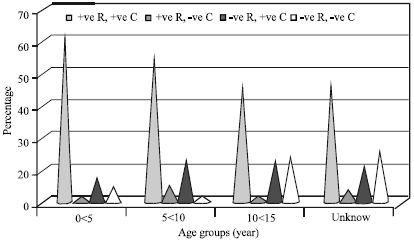
Development of an In-house ELISA for Detection of HCMV IgG and Finding of Antibody Avidity by Application of Diethylamine
Department of Virology, School of Medicine, Zahedan Medical University, Zahedan, Iran
P. J. Vallely
Department of Virology, School of Medicine, Manchester University, Manchester, UK