Review Article
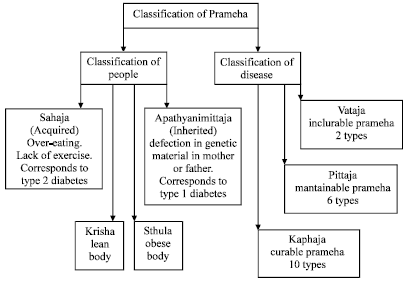
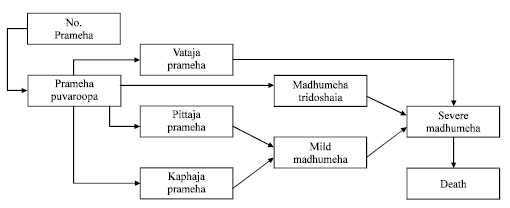
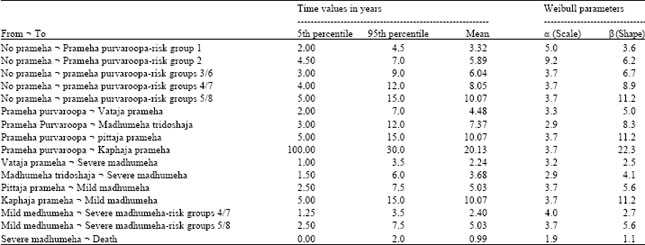
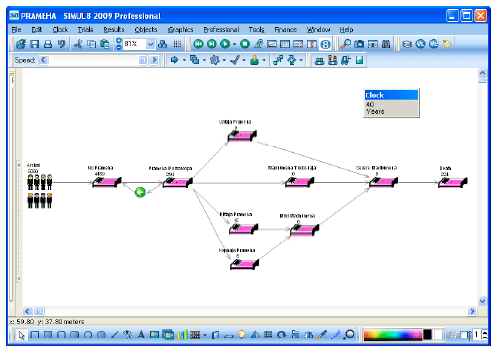
Computer Simulation Modelling for the Prevention of Diabetes Mellitus (Prameha)
Abeda Inamdar Senior College of Arts, Science and Commerce, Azam Campus, Camp, Pune-411 001, India
Arjan K. Shahani
GeoData Institute, University of Southampton, Southampton, SO17 1BJ, UK
Sanju Pal
Department of Mathematical Studies, University of Southampton, Southampton, SO17 1BJ, UK
Jyoti A. Shirodkar
Cheeranjiv Ayurveda Clinic, Bavdhan, Pune-411021, India
G. Gopal
Department of Statistics, University of Madras, Chennai-600 003, India