Research Article
Analysis of X-Ray Film Quality in Primary Health Care Clinics in Riyadh
Department of Radiological Sciences, College of Applied Medical Sciences, King Saud University, P.O. Box 10219, Riyadh 11433, Kingdom of Saudi Arabia
It is well known that diagnostic radiology is the major contributor to the total dose to the population from all artificial sources (UNSCEAR, 2000). Basic radiation protection principles require that safety and protection be optimized and that personal doses not exceed specific limits. They also require that the radiological examination must be justified and requested by a qualified individual (International Commission on Radiological Protection, 1991). In addition, international radiation protection regulations make it a requirement for all hospitals or clinics dealing with X-rays to ensure that the X-ray equipment and other related accessories are properly designed, installed and maintained. These regulations advocate the setting up and operation of a quality assurance program in such facilities. They also recommend the optimization of X-ray image in order to reduce the radiation dose to the patient (International Commission on Radiological Protection, 1996). The World Health Organization (1980) defined quality assurance programs in diagnostic radiology as an organized effort by the staff operating the facility to ensure that the diagnostic images produced in the facilities are of sufficiently high quality so that they consistently provide adequate diagnostic information at the lowest possible cost and with the least possible exposure of the patient to radiation.
The main purpose of the quality assurance program in a medical imaging department is to monitor the performance of all factors that could influence the quality of the image. This will result in reducing any film wastage within the department and minimizing the radiation exposure of patients and staff. Obtaining a satisfactory image can be achieved by correctly exposing and developing the x-ray film. Image quality can be tested by a technique known as sensitometry, which is a measure of the response of film density to exposure and development (McKinney, 1996). A curve known as 'characteristic curve' is obtained by plotting film densities against the log of relative exposure. This curve, also called H and D curve, carries a large amount of information on fog, gamma, contrast, average gradient, useful exposure range, useful density range, film latitude and speed (Gunn, 2002). The values of these variables from one set of films produced in one clinic or hospital can be analyzed and compared to those obtained from a control film. They can also be compared to values obtained from films produced in other clinics or hospitals.
Researchers have been carrying out studies to evaluate the image quality and to identify the possible causes of producing suboptimal images in diagnostic facilities. A report published in 2000 found that at least 20% of X-ray examinations in the United Kingdom were clinically useless for the management of patients. The report suggested that a quality assurance program is likely to play an important role in minimizing the number of rejected films (UNSCEAR, 2000).
Sniureviciute and Adliene (2005) studied problems with image quality in X-ray departments in Lithuania. They found that there was a lack of information about quality control of film processing. Staff members were not sufficiently aware of the necessity of quality control. The study also found that there was a lack of information on the number of rejected films and retakes. They recommended that institutions purchase and use equipment to control the developing process.
Rainford et al. (2007) evaluated four hospitals in Kuwait and Oman and compared them to 16 hospitals in the United Kingdom and the Republic of Ireland for the European Guidelines on Quality Criteria for Diagnostic Radiographic Images. They concluded that diagnostic quality of images was not always optimized across imaging sites.
As can be inferred from the previous studies, film processing is one of the most important factors influencing the quality of the radiographic image and the amount of radiation dose to the patient during X-ray examinations using screen-film technology. The purpose of this study was to inspect X-ray rooms in small primary health care clinics in Riyadh City. This study evaluated factors that affect the quality of radiographic images. Areas of non-compliance with international and local requirements were also identified. Suggestions were given on ways to improve the overall operation of X-ray rooms in these clinics.
The Ministry of Health (MOH) and King Abdul-Aziz City for Science and Technology (KACST) are responsible for quality control and radiation safety program implementation in hospitals and clinics in the country where ionizing radiations are used. Tertiary hospitals were not selected in this study as they have their own programs for quality control and radiation safety. In this study, 26 primary health care clinics having X-ray facilities were selected and surveyed between December 2006 and April 2007. The investigator has utilized the laboratory of the College of Applied Medical Sciences, King Saud University, for standardization of the testing equipment and techniques where fresh films were exposed and processed under standard conditions. The instruments used were a Sensitometer (Cardinal Health Dual Color Electronic Sensitometer-07-417) and a Densitometer (Cardinal Health Densitometer-07-443). Both were calibrated at the factory and gray scale strips were provided for checking and calibrating the equipment at the time of survey. The investigator also prepared a questionnaire to assess the different technical conditions in the facility. The main questions were related to the following issues:
| • | Whether the facility has ever been inspected by a qualified team for quality control |
| • | Whether a technologist, radiologist or any qualified person has ever carried out the quality control testing for the facility |
| • | Types of films, chemicals and film processor available |
The survey was started by physically checking the dark room, film and chemical storage facilities and the viewing area. The dark room was inspected for layout plan, film processor and safelight conditions, as well as exterior light leak through pass box, door or ventilation fan. Each clinic was evaluated on the above parameters as poor, good, very good, or N/A (Not available).
All clinics used automatic film processing units. These units were tested for performance, along with the types of films, cassettes and chemicals used. Films were taken from the film box available in each clinic and exposed by the sensitometer in the dark room and processed on the site. The optical density was measured for each tested film, a characteristic curve was plotted and radiographic parameters were calculated. The parameters used include: Base plus fog index, contrast index, speed index and maximum density level. They are calculated as follows:
| • | Base plus fog is obtained by measuring optical density from unexposed area of the film |
| • | Film contrast is the slope or rate of change of the curve within the range of useful densities (0.45-2.2 units) above base plus fog |
| • | Film speed is the reciprocal of exposure required to produce darkening of 1 unit above base plus fog value |
| • | The potential causes of abnormal variations in the above-mentioned parameters are discussed |
All of the 26 clinics in this study are administered by the Ministry of Health (General Directorate of Health Affairs). No radiologists are available in any of the clinics. Therefore, X-ray films are always read by the physicians (general practitioners). All clinics are equipped with basic X-ray units and have one radiographer with a radiography diploma certificate. In addition to operating the X-ray machine, the radiographer is also responsible for operation and day-to-day maintenance of the darkroom. None of the 26 clinics has ever been inspected by a qualified team other than the regular periodic inspection of the X-ray machine.
Darkroom facilities: The average number of films produced per examination was 1.2 and the average number of films used per clinic per month was 87 films. The study found that the cassettes in 95% (n = 25) of clinics were in good condition. The intensifying screens were without any defects or stains.
| Table 1: | Quality of dark-room facilities |
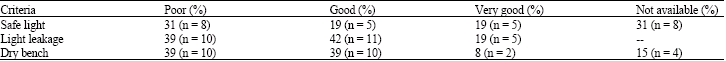 | |
| Table 2: | Types of processors, chemicals and X-ray films |
 | |
| Table 3: | Temperature setting of automatic processor |
 | |
The darkroom assessment results regarding safelight, light leakage and the availability of dry bench are shown in Table 1. Classification criteria used include very good, good and poor. Where very good means the facility is up to the standards, good means that there are some minor deficiencies but the room can still be used and poor means the room has major problems that are most probably affecting the quality of the image. As can be seen from Table 1, between 30 to 40% (n = 8-10) of the clinics are classified as poor in one or more criteria related to the dark room equipment. Of these, 31% (n = 8) did not have safelight and 15% (n = 4) did not have a dry bench for loading cassettes. Thirty nine percent of clinics (n = 10) had some kind of light leakage in the darkroom. All clinics used automatic processors that are mainly either Protec Compact-2 (Siemens), or AGFA. They used films and pre-mixed chemicals from either Kodak or AGFA (Table 2). Table 3 shows the temperature setting of the processors. The study has shown that 50% (n = 13) of clinics have temperature settings in the acceptable range (31-33°C). Fifteen percent (n = 4) of clinics had the setting below 30°C and 23% (n = 6) of them had the setting above 33°C. No temperature indicator was available in the processors of 12% (n = 3) of clinics (Table 3).
H and D curve analysis: Characteristic curves calculated from films produced in the 26 clinics are shown in Fig. 1 and 2. From these curves, base plus fog index, contrast index, speed index and maximum density are calculated and compared to the control (Table 4). Table 4 shows that base plus fog indexes are within normal range in only 23% (n = 6) of clinics, whereas 50% (n = 13) of clinics have values above and 27% (n = 7) have values below the normal range. The contrast index has also shown large variations compared to the control. In this case only 35% of clinics (n = 9) are within the normal range whereas the rest are either above (46% (n = 12)), or below (19% (n = 5)) this range.
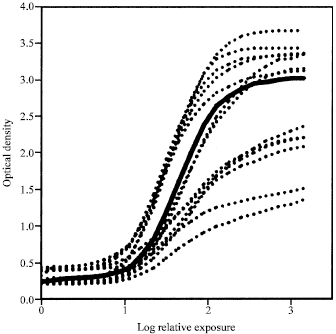 | |
| Fig. 1: | H and D Curve (clinic 1 to 13) (Slid line = Control) |
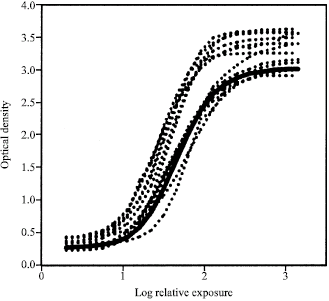 | |
| Fig. 2: | H and D Curve (clinic 14 to 26) (Slid line = Control) |
The same table also shows that the film speed index is within the normal range in only 46% of clinics (n = 12).
| Table 4: | H and D curve analysis |
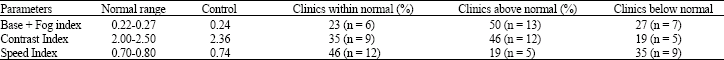 | |
Regular quality control has been shown to improve the performance of X-ray units, which then results in improving image quality as well as reducing radiation doses to patients and staff (Bosnjak et al., 2008). This study was conducted to determine the factors influencing image quality in primary health care clinics located in Riyadh City. The author demonstrated a relationship between the results of the H and D curve analysis and the factors known to affect image quality. These factors include: film type, film and chemical storage conditions and film processing. It is important to mention here that although a film may not pass the standard image quality measures, it may still have a diagnostic value in general practice, where only routine radiography is performed. Also, since few of the clinics do more than 5-10 films per day, following strict quality control measures may be unpractical.
The majority of films produced in the surveyed clinics are considered unsatisfactory in one or more of the image quality parameters. The low quality of the darkroom and processing conditions are the major causes of the reduced image quality. For instance, the increase in base plus fog density values in about 50% of the clinics, despite the fact that cassettes and films are new and of good quality, indicates that storage conditions of films and chemicals, as well as the quality of the darkroom safe light are not properly maintained. Haus and Jaskulsi (1997) reported similar results where they showed that storage conditions of both films and chemicals can affect the quality of X-ray films.
Process-related artifacts, that include excessive film fog and lower contrast index values, are caused either by the inaccurate setting of the processor temperature control or poor replenishment of chemicals. Studies have shown that these artifacts can be minimized by performing basic quality control measures on the processor at the beginning of each day (Hogge et al., 1999). In addition, some clinics may not be using film types that match the type of screens mounted in the cassettes, resulting in lower speed and lower contrast. The radiographer in this case has to increase the exposure factors in order to compensate for this decrease in optical density. This will result in giving the patient a higher dose of radiation (Suleiman et al., 1992).
The deficiencies mentioned above are also the reason for the increase in the percentage of film rejection rate in surveyed clinics as shown by Aghahadi et al. (2006). On average, about 5-10% of total films taken are rejected, resulting again in exposing the patient to unnecessary radiation and wasting public time and resources.
In conclusion, this study shows that taking simple measures regarding film processing can substantially improve image quality. Such measures include performing the basic regular maintenance of darkroom equipment, proper adjustment of processor temperature, prevention of light leakage in the darkroom, storing films and chemicals in a proper environment and the use of right film-screen combination. A well trained radiographer is capable of performing these tasks and thus improving image quality in small clinics where major quality control tests may not be practical.
The author would like to thank Dr. S.C. Kapur and Mr. Emadeldin A. Ali Bashir from the College of Applied Medical Sciences, King Saud University for assisting with data analysis. The author also would like to thank the Ministry of Health in Saudi Arabia (General Directorate of Health Affairs in Riyadh Region) for granting the permission and facilitating the conduction of the survey. This study was supported in part by King Saud University, Riyadh, Saudi Arabia.