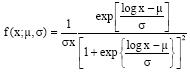Research Article
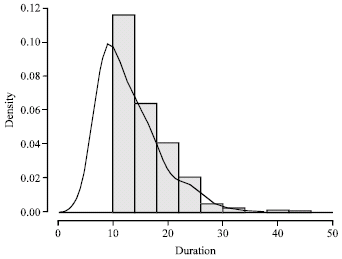
Modelling the Duration of Hypopnea
Department of Biomedical Sciences, Faculty of Allied Health Sciences, University Kebangsaan Malaysia, 50300 Jln Raja Muda Abdul Aziz, Kuala Lumpur, Malaysia
Abdul Aziz Jemain
School of Mathematical Sciences, Faculty of Science and Technology, Universiti Kebangsaan Malaysia, 43600 Bangi, Selangor DE, Malaysia