Research Article
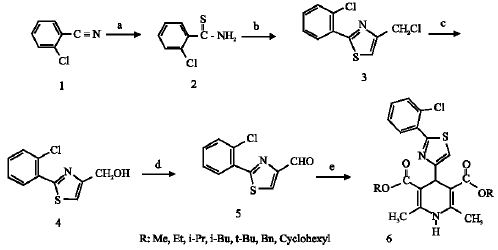
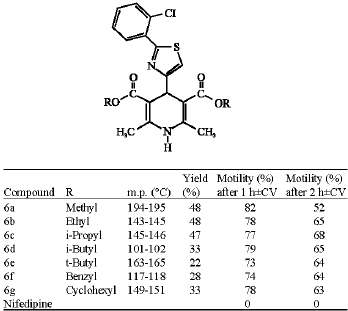
Synthesis of Dihydropyridine Analogues for Sperm Immobilizing Activity
1Department of Physiology, Faculty of Medicine, Tehran University of Medical Sciences, Tehran, Iran
M. Amini
2Department of Medicinal Chemistry, Faculty of Pharmacy and Pharmaceutical Sciences Research Center, Tehran University of Medical Sciences, Tehran, Iran
Z. Naghibi Harat
1Department of Physiology, Faculty of Medicine, Tehran University of Medical Sciences, Tehran, Iran
P. Daneshgar
2Department of Medicinal Chemistry, Faculty of Pharmacy and Pharmaceutical Sciences Research Center, Tehran University of Medical Sciences, Tehran, Iran
M. Vosooghi
2Department of Medicinal Chemistry, Faculty of Pharmacy and Pharmaceutical Sciences Research Center, Tehran University of Medical Sciences, Tehran, Iran
A. Shafiee
2Department of Medicinal Chemistry, Faculty of Pharmacy and Pharmaceutical Sciences Research Center, Tehran University of Medical Sciences, Tehran, Iran