Research Article
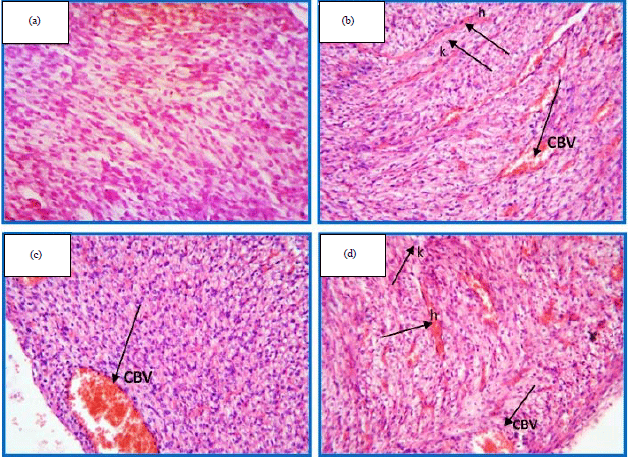
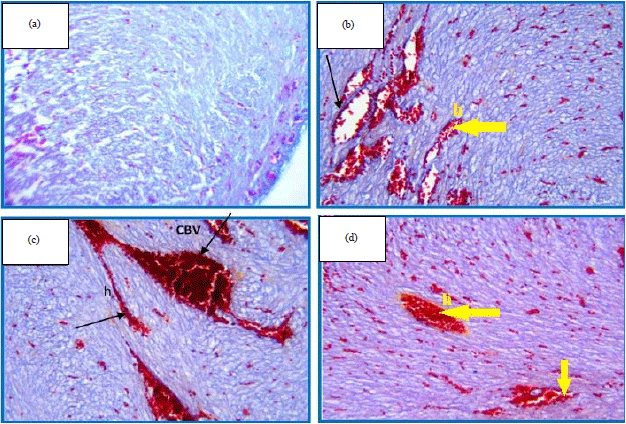
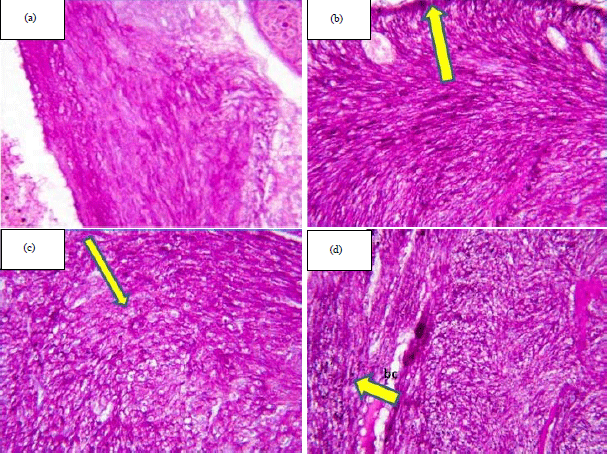
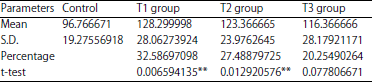
Histological and Histochemical Alternations in the Fetal Heart Tissue of Maternal Prozac Exposure
Biology Department, College of Science, Jouf University, P.O. Box 2014, Sakaka, Saudi Arabia
LiveDNA: 20.22576
Khadija Abdul Jalil Faddladdeen
Faculty of Science, King Abdul Aziz University, Saudi Arabia