Research Article
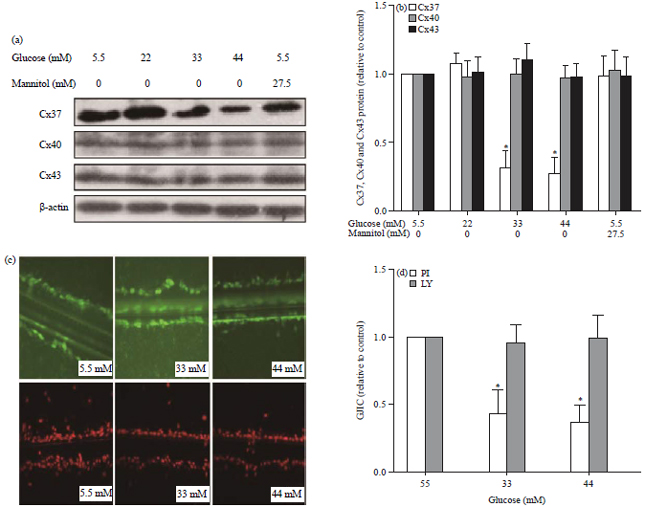
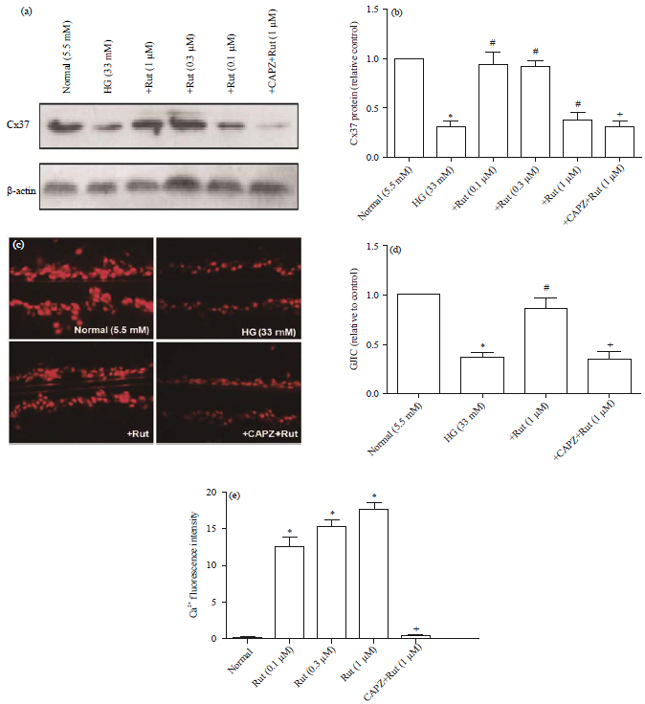
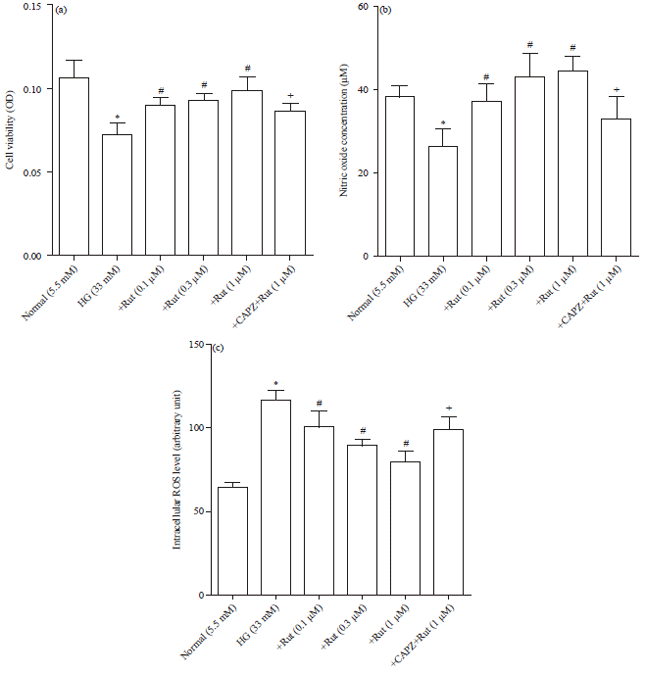
Rutaecarpine Prevents High Glucose-induced Cx37 Gap Junction Dysfunction in Human Umbilical Vein Endothelial Cells
Department of Physiology, Medical School, Nanchang University, Bayi Road 461, 330006 Nanchang, Jiangxi Province, People`s Republic of China
Hang Yan
Department of Physiology, Medical School, Nanchang University, Bayi Road 461, 330006 Nanchang, Jiangxi Province, People`s Republic of China
Yan Zhao
Department of Physiology, Medical School, Nanchang University, Bayi Road 461, 330006 Nanchang, Jiangxi Province, People`s Republic of China
Yanrong Yu
Jiangxi Academy of Medical Sciences, Bayi Road 461, 330006 Nanchang, Jiangxi Province, People`s Republic of China
Haibing Kuang
Department of Physiology, Medical School, Nanchang University, Bayi Road 461, 330006 Nanchang, Jiangxi Province, People`s Republic of China
Qiren Huang
Department of Pharmacology, Fuzhou Medical College, Nanchang University, Dongling Road 9, 344000 Fuzhou, Jiangxi Province, People`s Republic of China
Ming He
Department of Pharmacology, Fuzhou Medical College, Nanchang University, Dongling Road 9, 344000 Fuzhou, Jiangxi Province, People`s Republic of China
Dan Luo
Department of Physiology, Medical School, Nanchang University, Bayi Road 461, 330006 Nanchang, Jiangxi Province, People`s Republic of China
LiveDNA: 86.20650
Weijie Peng
Key Provincial Laboratory of Basic Pharmacology, Nanchang University, Bayi Road 461, 330006 Nanchang, Jiangxi Province, People`s Republic of China