Research Article
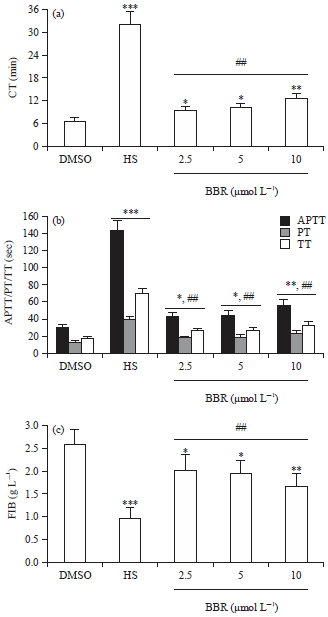
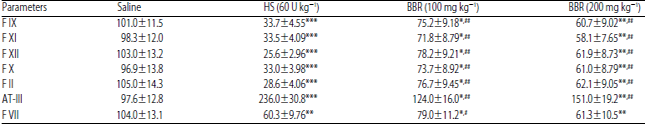
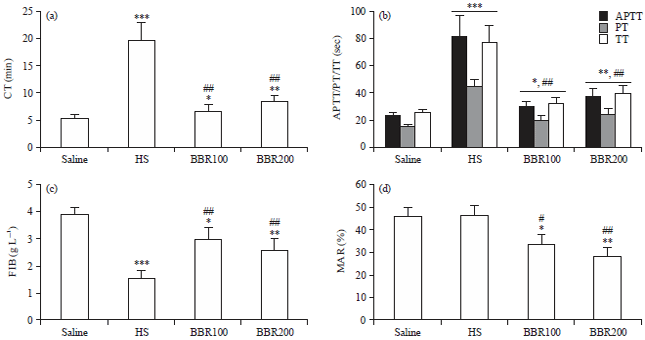
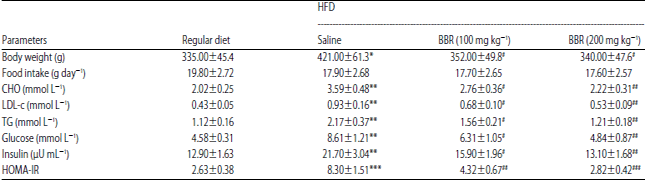
Evaluation of Anticoagulant and Antithrombotic Activities of Berberine: A Focus on the Ameliorative Effect on Blood Hypercoagulation
New Drug Safety Evaluation Center, Institute of Materia Medica, Chinese Academy of Medical Sciences and Peking Union Medical College, 100050, Beijing, China
Yan-Bin Wu
Department of Virology, Institute of Medicinal Biotechnology, Chinese Academy of Medical Sciences and Peking Union Medical College, Beijing ,100050, China
Ai-Ping Wang
New Drug Safety Evaluation Center, Institute of Materia Medica, Chinese Academy of Medical Sciences and Peking Union Medical College, 100050, Beijing, China
Jian-Dong Jiang
State Key Laboratory of Bioactive Natural Products and Function, Institute of Materia Medica, Chinese Academy of Medical Sciences and Peking Union Medical College, 100050, Beijing, China
Wei-Jia Kong
Department of Virology, Institute of Medicinal Biotechnology, Chinese Academy of Medical Sciences and Peking Union Medical College, Beijing ,100050, China
LiveDNA: 86.24126