Research Article
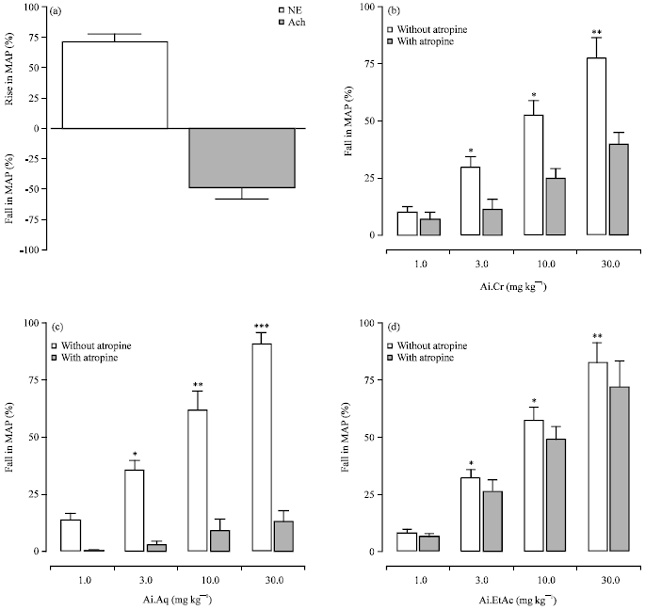
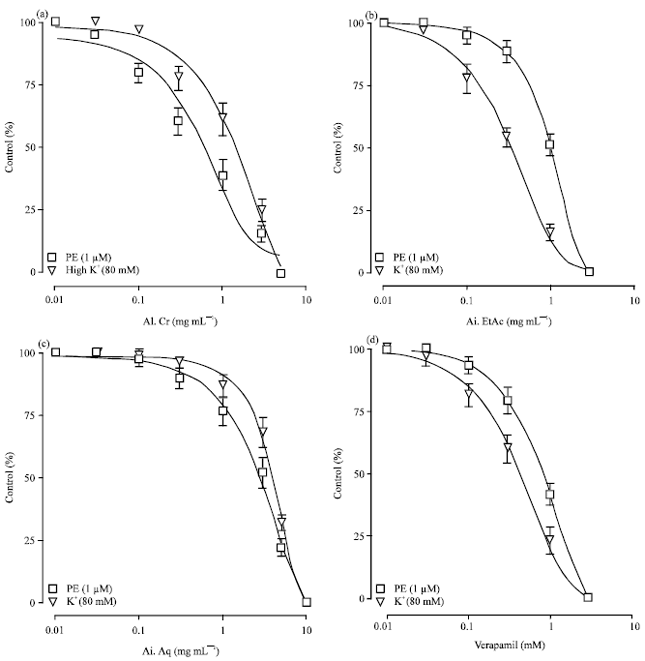
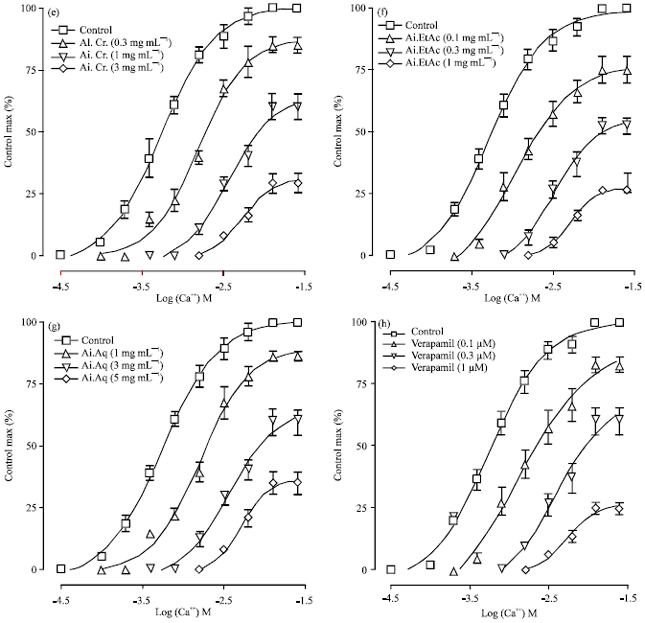
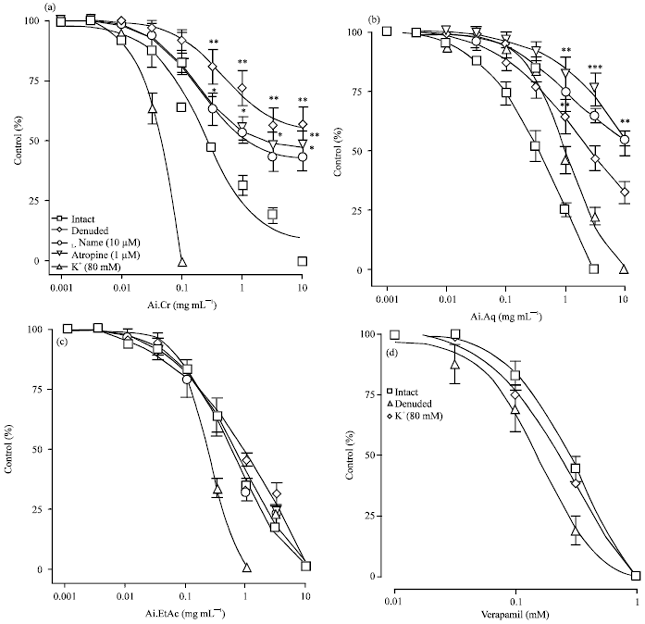
Neem (Azadirachta indica) Lowers Blood Pressure through a Combination of Ca++ Channel Blocking and Endothelium-Dependent Muscarinic Receptors Activation
Department of Biological and Biomedical Sciences, Natural Products Research Division, Aga Khan University Medical College, Karachi, 74800, Pakistan
Anwarul-Hassan Gilani
Department of Biological and Biomedical Sciences, Natural Products Research Division, Aga Khan University Medical College, Karachi, 74800, Pakistan
Hashim Muhammad Hanif
Department of Biological and Biomedical Sciences, Natural Products Research Division, Aga Khan University Medical College, Karachi, 74800, Pakistan
Saeed Ahmad
Department of Biological and Biomedical Sciences, Natural Products Research Division, Aga Khan University Medical College, Karachi, 74800, Pakistan
Sana Khalid
Department of Biological and Biomedical Sciences, Natural Products Research Division, Aga Khan University Medical College, Karachi, 74800, Pakistan
Ishfaq A. Bukhari
Department of Pharmacology, College of Medicine, King Saud University, Riyadh, Saudi Arabia