Research Article
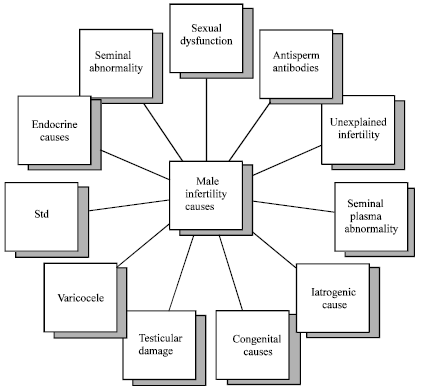
Male Infertility in Bangladesh: What Serve Better-Pharmacological Help or Awareness Programme?
Infertility Treatment Research Center, Mohammadpur, Dhaka 1207, Bangladesh
Gazi Mahabubul Alam
Academic Performance Enhancement Unit, University of Malaya, Jalan Panati Baharu, 59990 Kuala Lumpur, Malaysia
M.A. Kabir
Faculty of Economics and Administration, University of Malaya, 50603 Kuala Lumpur, Malaysia
Abul Quasem Al-Amin
Faculty of Economics and Administration, University of Malaya, 50603 Kuala Lumpur, Malaysia











Md. Saiful Islam Reply
I am Patient of azoospermia. my conjugal life is 12 years.My age 44 years & Wife 38 year sold. I have testing fnac pg hospital result Normal spermatagenisbut seman analysis report nill. others hormonal test is ok.
now iam diabeties patient from 6 years. Iam engaged in private job stay Gazipur. We always expect for a Baby. we take medicine many doctor advice But no result.So Can I help by you & yours.
Mostafizur Rahman Shah Reply
I am Patient of azospermia . My conjugal life is 12 years. My age is 37 years & my wife is also 37 years old. I tested my semen on 2011 & found sperm mortality 80% during this period my wife's menstruation was irregular. In 2013 she completed a laporoscopy under Prof. T. A Chowdhury. From last 1 year her menstruation is regular.Now I am a diabetic patient from last 4 months.Now my sperm mortality is 10% (October,20,2014) I am engaged in a private job & from Rajshahi. We always expect for a Baby. Would you enough please to help us regarding our treatment. Can we be a parents?
Mohammad Kamruzzaman Reply
Dear Sir,
I have a azoospermia. My Blood Condition is so poor. Mr. Doctor is not Interested doing the test TESA. Becoz. Now my Blood Condition is Testosterone Leve...is 6.7 noml/L & FSH is 19.6 Ul/L. So, What can i do.& tell me what % of Successes? If you have a any treatment to get the baby.
I am waiting for you replay soon.