Research Article
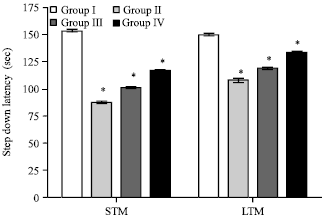
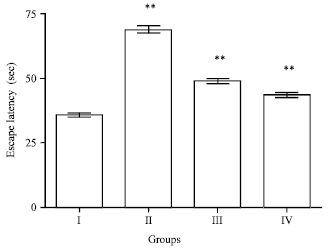
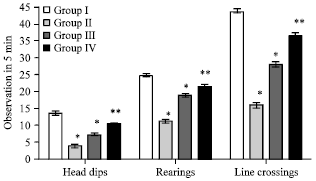
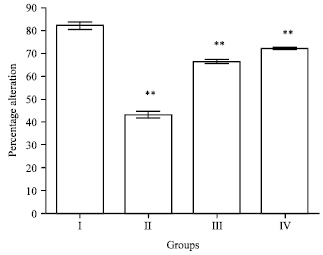
Ameliorating Effect of Ethanol Leaf Extract of Ficus hispida Linn. on Amyloid beta Aβ (25-35) Induced Cognitive Deficits and Oxidative Stress in Alzheimer’s Mice
Department of Pharmacology and Toxicology, C.L. Baid Metha College of Pharmacy, Jyothi Nagar, Thoraipakkam, Chennai 97, Tamil Nadu, India
P. Muralidharan
Department of Pharmacology and Toxicology, C.L. Baid Metha College of Pharmacy, Jyothi Nagar, Thoraipakkam, Chennai 97, Tamil Nadu, India
P. Panneerselvam
Department of Pharmaceutical Chemistry, C.L. Baid Metha College of Pharmacy, Jyothi Nagar, Thoraipakkam, Chennai 97, Tamil Nadu, India