Research Article
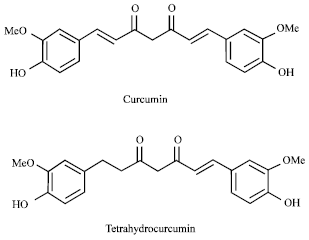
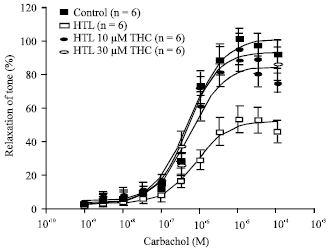
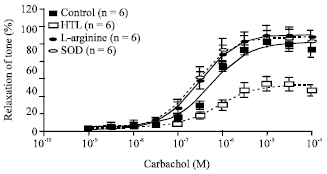
Curcumin and Tetrahydrocurcumin Restore the Impairment of Endothelium-dependent Vasorelaxation Induced by Homocysteine Thiolactone in Rat Aortic Rings
Department of Physiology, Faculty of Medicine, Srinakharinwirot University, Bangkok 10110, Thailand
A. Suksamrarn
Department of Chemistry, Faculty of Science, Ramkhamhaeng University, Bangkok 10240, Thailand