Research Article
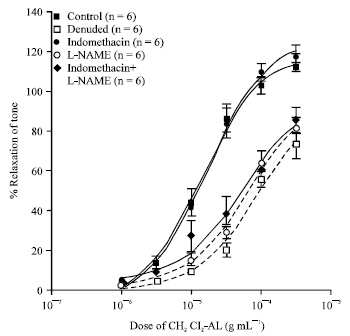
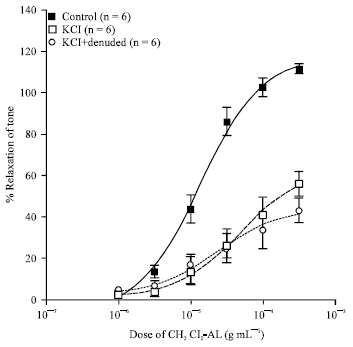
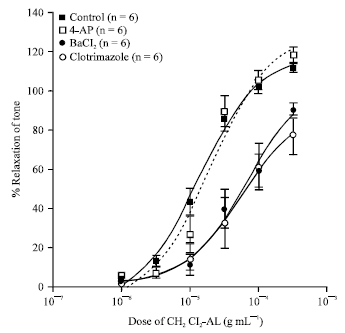
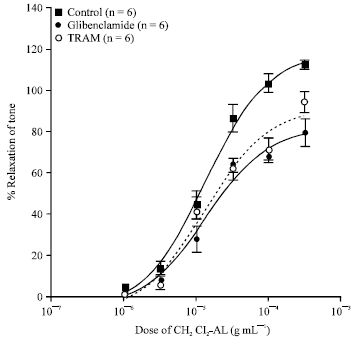
The Vasorelaxant Effects of Anaxagorea luzonensis A. Grey in the Rat Aorta
Department of Physiology, Faculty of Medicine, Srinakharinwirot University, Bangkok 10110, Thailand
P. Sawasdee
Natural Products Research Unit, Department of Chemistry, Faculty of Science, Chulalongkorn University, Bangkok 10330, Thailand