Research Article
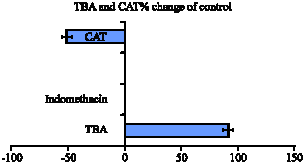
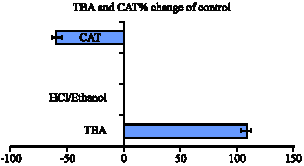
Chloroquine Phosphate Potentiates Indomethacin and HCl/Ethanol-Induced Gastric Mucosa Injury in Rats
Department of Physiology, School of Basic Medical Sciences, Igbinedion University, Benin City, Nigeria
E.O. Nwobodo
Department of Physiology, Faculty of Medicine, Nnamdi Azikiwe University, Nnewi, Nigeria
T.O. Oyesola
Department of Physiology, School of Basic Medical Sciences, Igbinedion University, Benin City, Nigeria
D.A. Ofusori
Department of Anatomy, School of Basic Medical Sciences, Igbinedion University, Benin City, Nigeria
S.B. Olaleye
Department of Physiology, College of Medicine, University of Ibadan, Ibadan, Nigeria