Research Article
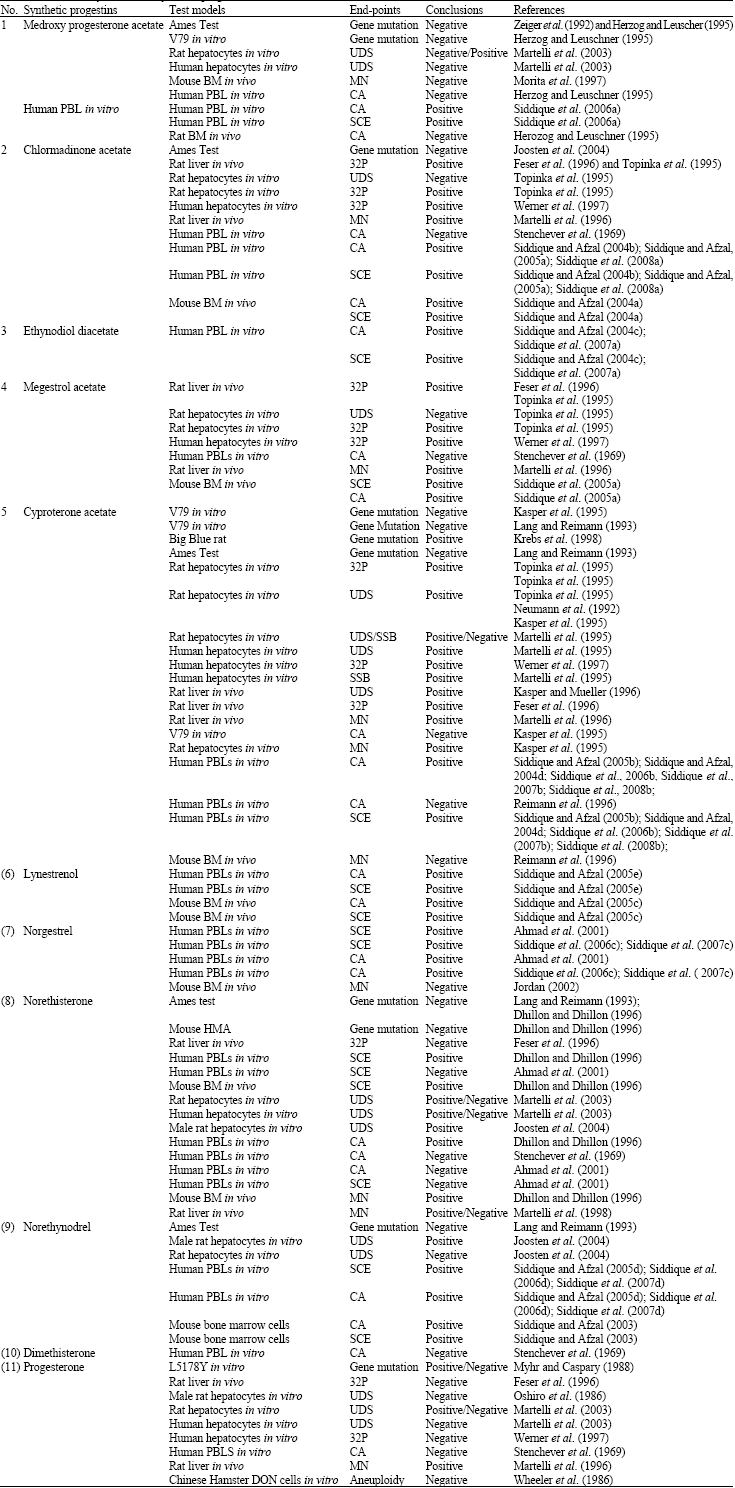
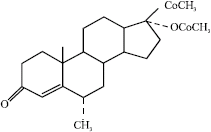
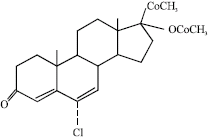
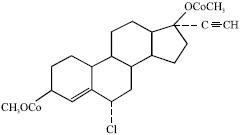
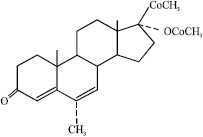
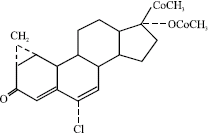
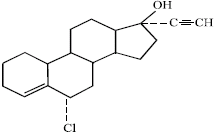
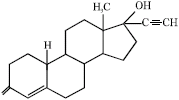
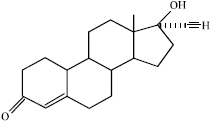
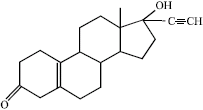
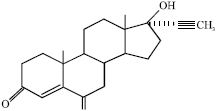
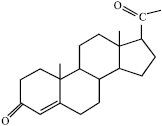
A Review on the Genotoxic Effects of Some Synthetic Progestins
Human Genetics and Toxicology Laboratory, Section of Genetics, Department of Zoology, Faculty of Life Sciences, Aligarh Muslim University, Aligarh (UP)-202002, India
M. Afzal
Human Genetics and Toxicology Laboratory, Section of Genetics, Department of Zoology, Faculty of Life Sciences, Aligarh Muslim University, Aligarh (UP)-202002, India