Research Article
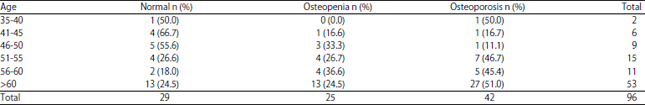
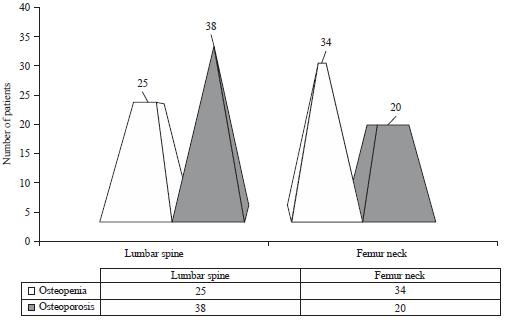
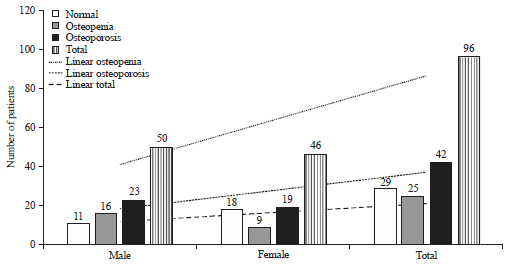
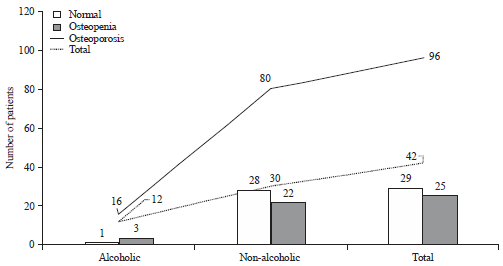
Prevalence of Osteoporosis in Type 2 Diabetes Mellitus Patients Using Dual Energy X-Ray Absorptiometry (DEXA) Scan
Department of Orthopaedics, KLE University`s JN Medical College, Nehru Nagar, 590010 Belagavi, India
Ravi. S. Jatti
Department of Orthopaedics, KLE University`s JN Medical College, Nehru Nagar, 590010 Belagavi, India
Shridhar C. Ghagane
Department of Diabetology and Medicine, KLES Diabetes Centre, KLES Dr. Prabhakar Kore Hospital and Medical Research Centre, JN Medical College, KLE Academy of Higher Education and Research (KLE University) Nehru Nagar, 590010 Belagavi, Karnataka, India
S.M. Jali
Department of Diabetology and Medicine, KLES Diabetes Centre, KLES Dr. Prabhakar Kore Hospital and Medical Research Centre, JN Medical College, KLE Academy of Higher Education and Research (KLE University) Nehru Nagar, 590010 Belagavi, Karnataka, India
M.V. Jali
KLE Academy of Higher Education and Research (KLE University), Nehru Nagar, 590010 Belagavi, India
LiveDNA: 91.16811