Research Article
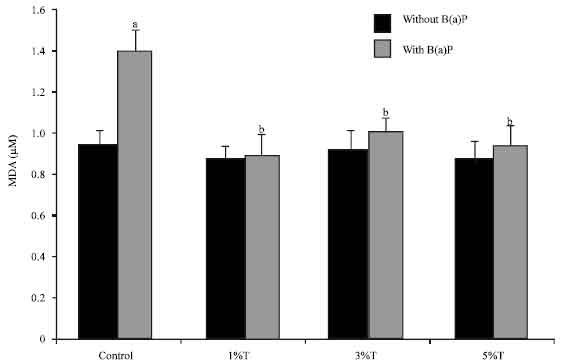
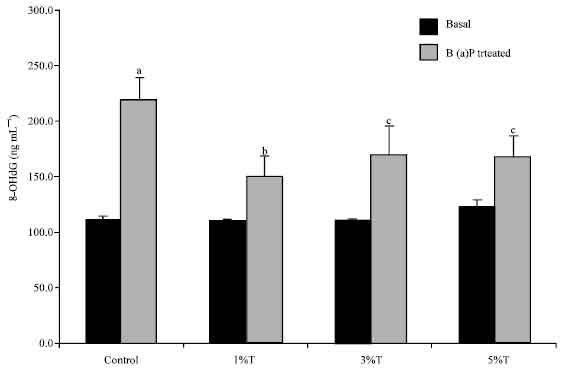
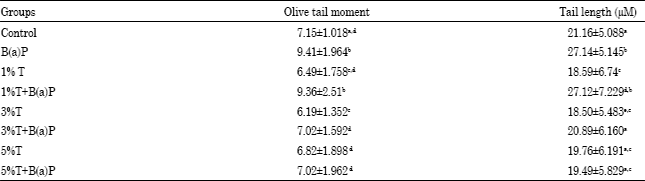
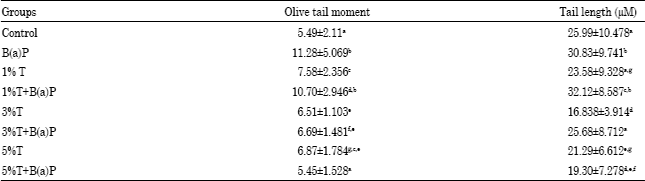
Turmeric Alleviates Benzo(a)pyrene Induced Genotoxicity in Rats: Micronuclei Formation in Bone Marrow Cells and DNA Damage in Tissues
Food and Drug Toxicology Research Centre, National Institute of Nutrition, Indian Council of Medical Research, Hyderabad-500 007, India
Virendra V. Panpatil
Food and Drug Toxicology Research Centre, National Institute of Nutrition, Indian Council of Medical Research, Hyderabad-500 007, India
A.K. Raja Kumar
Food and Drug Toxicology Research Centre, National Institute of Nutrition, Indian Council of Medical Research, Hyderabad-500 007, India
N. Balakrishna
Department of Statistics, National Institute of Nutrition, Indian Council of Medical Research, Hyderabad-500 007, India
R. Balansky
National Specialized Hospital for Active Treatment of Cancer, Str. Plovdivsko pole 6, Sofia-1756, Bulgaria, India
K. Polasa
Food and Drug Toxicology Research Centre, National Institute of Nutrition, Indian Council of Medical Research, Hyderabad-500 007, India