Research Article
Palliative Small Bowel Surgery in Patients with History of Malignancy
Department of Surgery Auckland Hospital, Grafton, Auckland, New Zealand
A.E. Merrie
Department of Surgery Auckland Hospital, Grafton, Auckland, New Zealand
Bowel obstruction in patients with history of cancer is caused by recurrence of malignant disease in 50% of the cases (Agrawal et al., 1999) (Walsh and Schofield, 1984). In patients with previously treated colorectal cancer with curative intent 10% develop small bowel obstruction, half of them are due to recurrence (Walsh and Schofield, 1984). Small bowel obstruction due to recurrent intra or extra abdominal cancer is commonly caused by colorectal cancer, ovarian malignancies and malignant melanoma (Butler et al., 1991; Ellis et al., 1991; Miller et al., 2000). Small bowel obstruction due to recurrent cancer tends to happen earlier (within two years after the initial surgery) than obstruction caused by band adhesions, which have a median time of occurrence of 5 years after the original surgery (Butler et al., 1991).
Small bowel obstruction secondary to recurrent cancer carries a grim outlook, however surgical intervention offers better palliation to reduce symptoms and was shown to reduce re-obstruction rates (Miller et al., 2000). Although it is associated with high morbidity and mortality rates, surgical intervention is generally recommended as the best palliation in such patients (Ellis et al., 1991; Fletcher, 2002).
Long-term survival is variable and the important factors are poorly identified. We conducted this study to assess factors that affect long-term survival, which may help in prognostication and management of those patients.
Auckland Hospital data was searched for the period 1992-2003 for patients who had small bowel resection for cancer in patients who had previously treated cancer regardless of the primary site. Data collected by reviewing patients’ files include demographics, primary cancer and interval to occurrence of small bowel involvement, overall morbidity and mortality and length of survival after small bowel resection.
Overall survival was calculated and univariate analysis (using Pearson correlation test) was performed to correlate survival with primary diagnosis, interval to recurrence and extent of intra-abdominal disease. Log rank test was used to compare survival difference between different groups. Multivariate analysis was performed using the Cox regression hazard model to specify factors that have impact on overall survival. Statistics were performed using SPSS 11.5 for windows.
Between 1992-2003, 79 patients [(34 males) (median age 62, range 19-91)] had laparotomy with or without small bowel resection for small bowel obstruction due to intra-abdominal spread of previously treated intra or extra abdominal cancer (Table 1). The most common cause was colorectal cancers followed by gynecologic malignancies and melanoma; others were related to breast (5), stomach (3), lung (1), prostate (2) and kidney (1). Diffuse intra abdominal disease was found in 59 patients and 20 patients had limited and resectable disease which was completely removed. Overall complication rate was 35% and 8 (10%) patients died. Median overall survival was 5 months (Fig. 1).
Overall survival correlates with type of the primary cancer and extent of intra abdominal metastases (p = 0.03, Pearson correlation test), patients with primary diagnosis of colorectal cancer tend to have slightly less intra peritoneal disease burden and better overall survival than other types of malignancies (median of 7 months vs. 4 moths, p = 0.02) (Fig. 2).
Cox regression model of multivariate analysis was used to compare factors that affect overall survival; it showed that among factors that can possibly influence survival, extent of intra-peritoneal disease is the only factor that have an important impact on survival, median survival for patients with limited resectable disease was 17 months compared with 4 months for unresectable disease, (p = 0.002).
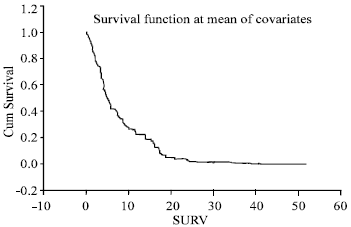 | |
| Fig. 1: | Overall survival for all patients, fraction of patients against months |
| Table 1: | Survival by primary malignancy |
 | |
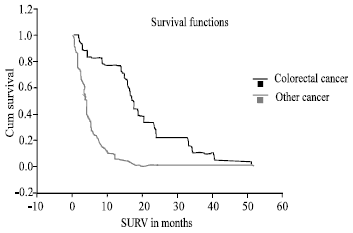 | |
| Fig. 2: | Survival difference between colorectal cancer and other cancers (log rank test). fraction of patients against months |
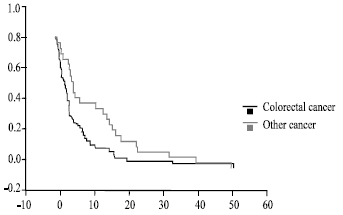 | |
| Fig. 3: | Survival by the extent of the disease. Fraction of patients against months |
Age, primary diagnosis and time interval between the diagnosis of the primary and the recurrence have no effect on survival (Fig. 3).
This study is a retrospective review of 12 years experience in malignant small bowel obstruction. We found that the commonest cause of recurrent malignant small bowel obstruction is colorectal cancer followed by gynecologic cancers and malignant melanoma. Malignant melanoma was the commonest extra-abdominal cancer to cause abdominal metastasis resulting in small bowel obstruction; among other cancers it has the longest interval between primary treatment and recurrence (median of 5 years). Surgery offered a median survival of 7 months with best results in patients with primary diagnosis of colorectal cancer and those with isolated intra-abdominal metastases where complete macroscopic clearance of the disease was possible. The multivariate analysis shows that extent of recurrent disease as the only factor that affects duration of overall survival. Although patients with colorectal cancer had better overall survival this may reflect the fact that it is more likely than other cancers to have respectable disease.
Operative mortality has been reported as significantly high in particular in patients who present urgently with tumor recurrence causing acute small bowel obstruction, Walsh reported 19% death rate (Fletcher et al., 2002), Butler et al. (1991) reported 24% 30 days mortality. Very high death rates of 67% were reported after emergency laparotomy. Surgical intervention in those patients is associated with a significant complications rate; wound complications, intra-abdominal sepsis and cardio-pulmonary complications are the commonest postoperative complications (Butler et al., 1991). Overall complications rate varies from 8% in patients with melanoma (Agrawal et al., 1999) to 44% in gynecologic malignancies (Blair et al., 2000) . Median overall survival varies from 5-11months (Tang et al., 1994; Walsh and Schofield, 1984; Makela et al., 1990). The longest survival is reported in patients with metastatic malignant melanoma by Agrawal et al. (1999) that described median survival after complete resection of 15 months with 38% 5 years survival. Malignant melanoma was associated with the longest interval between diagnosis of the primary and appearance of abdominal metastastasis. Patients with colorectal primary seem to have better outcome than other causes with overall survival up to 2 years (Tang et al., 1990) most patients have disease recurrence within 2 years of resection of the primary colorectal cancer (Blair et al., 2000).
Currently there is no universally accepted method of imaging follow up with view of detecting recurrence in patients with colorectal or ovarian cancers. Tumor markers such as CEA for colorectal cancer and CA 125 for ovarian cancer are useful tool, however that does not accurately define the timing of recurrence neither it quantifies the extent of the disease. CT scan and contrast enhanced CT colonography are useful tools for detection of recurrent colorectal and ovarian and other cancers (Miller et al., 2000; Chau et al., 2004; Bristow et al., 2003). PET is promising tool for early detection of recurrent intra-abdominal cancer when tumors makers are elevated in a symptomatic patient with no signs of recurrence on CT imaging (Simo et al., 2002; Chau et al., 2004; Fletcher et al., 2002; Flamen et al., 2001; Miller et al., 2004) this modality is not yet widely available future availability of this tool may increase the rate of early detection of recurrent disease at stages when it is resectable.
In conclusion recurrence should be suspected in patients with history of malignancy who present with small bowel obstruction, CT scan is useful to localize the site of obstruction and to assess the presence of recurrent disease and its extent. Aggressive surgical management is recommended in those who prove to have resectable recurrence, however such intervention has to weighed against an expected high complications and mortality rate. Every effort should be made to pursue conservative approach in those who have non-removable recurrence. Future efforts are to be directed for development of strategies for early detection of intra-abdominal recurrence or metastases.