ABSTRACT
Limited research has been done to assess the effectiveness of Muscle Energy Technique (MET) on Temporomandibular Joint Dysfunction (TMD) patients. The present study was a randomized clinical trial that aimed to evaluate the effectiveness of MET in reducing pain and improving Maximal Mouth Opening (MMO) in patients with TMD. The sample consisted of forty participants; aged 20-30 years (mean age 25.5±2.96) diagnosed with TMD of less than three months duration were recruited. Participants were treated with MET, which includes post isometric relaxation and reciprocal inhibition, given on alternate days for 5 weeks. Before the commencement of the treatment and at the end of each week, subjects were evaluated for pain intensity using Visual Analogue Scale (VAS) and MMO by measuring the inter-incisal distance. The intra group comparison showed that there was a significant reduction of pain (p<0.05) at the end of each week as measured by the VAS. The MMO measurements showed significant improvement in range of motion (p<0.05) at the end of each week when compared to the baseline measurements. Results may have important implications for physiotherapy practice in suggesting that MET is effective in reducing pain and improving MMO in patients with TMD.
PDF Abstract XML References Citation
How to cite this article
DOI: 10.3923/ajsr.2011.71.77
URL: https://scialert.net/abstract/?doi=ajsr.2011.71.77
INTRODUCTION
Temporomandibular joint dysfunction (TMD), is an umbrella term for a group of pathologies affecting the masticatory muscles, the temporomandibular joint (TMJ) and its related structures (McNeil, 1993; Di Fabio, 1998). Although, traditionally viewed as a syndrome, the recent studies supports that TMD is a cluster of related disorders in the masticatory system, which has many common features (Bell, 1990; Griffiths, 1983). The term has been used synonymously with a host of other terms including TMJ disorders, TMJ dysfunction syndrome, craniomandibular disorders and myofascial pain dysfunction syndrome (Yap and Ho, 1999). TMD is considered a musculoskeletal disorder of the masticatory system that affects more than 25% of the general population (Gremillion, 2000). An estimated 85 to 95% of the population will exhibit one or more symptoms of TMD in their lifetime (Saghafi and Curl, 1995) with 5 to 6% of the population reporting clinically significant TMD related jaw pain (Goulet et al., 1995).
Cross sectional epidemiological studies in specific population showed that about 75% have at least one sign of joint dysfunction (tenderness, joint sounds etc.) and about 33% have at least one symptom (face pain, joint pain, muscle pain etc.) (Rugh and Solberg, 1985; Schiffman and Fricton, 1988). Clinical population studies have, however shown that a smaller percentage of people have problems severe enough to seek care for TMD and those who sought treatment included more women than men by about 8:1 (Rugh and Solberg, 1985). TMD accounts for a large percent of non dental pain in the oro-facial region, with pain being one of the most frequently presenting symptoms (Yap et al., 2002), usually involving the muscles of mastication (temporalis, masseter and the medial and lateral pterygoids), the pre-auricular area and/or the temporomandibular joint.
TMD has a wide range of symptoms including restricted range of mouth opening, locking, clicking and commonly joint and muscle pain (De Wijer et al., 1996). It is also commonly associated with other features affecting the head and neck regions such as headache, ear-related symptoms and cervical spine disorders (Gremillion, 2000; Rocabado, 1987). Patients with chronic TMD frequently report of depression, poor sleep quality and low energy (Morris et al., 1997). Further, chronic TMD has been found to interfere with normal social activity and interpersonal relationships and negatively affect the ability to maintain employment (Morris et al., 1997).
Management of TMD often involves a multidisciplinary approach; dentists, orthodontists, physical therapists, physicians and psychologists work together (McNeil, 1993). Conservative treatment is considered to be the treatment of choice because of the symptomatology of the condition is often improved by use of occlusal splints, physical therapy, medication and orthodontic treatment (Friction and Dubner, 1995). Current treatment of TMD includes pharmacological intervention, behaviour modification, nutritional counselling, occlusal therapy, physical therapy and manual therapy, orthodontics, prosthetics, orthotics and surgery. Considering the complexity of TMD, certain patients may benefit from more than one treatment modality at any one time (Gosling and Frois, 2004).
Numerous physical therapy interventions are potentially effective in managing TMD, including electrophysical modalities, exercise and manual therapy techniques. Electrophysical modalities include interventions such as ultrasound, microwave, laser and TENS (McNeil, 1993). Physical therapy interventions often include therapeutic exercises for the masticatory or cervical spine muscles to improve strength and mobility in the region (Rocabado, 1987). Manual therapy techniques are commonly used to reduce pain and restore mobility (McNeil, 1993). The more popular and widely used manual therapy techniques in the management of musculoskeletal disorders are the Maitland mobilization technique and Muscle energy technique.
Muscle Energy Techniques (MET) are used to treat muscles with excessive tension, which limit joint motion and cause pain (Chiatow, 2006). MET can be used to lengthen a shortened or spastic muscle and to strengthen a physiologically weakened muscle to reduce localized oedema and to relieve passive congestion (Greenman, 1996). Treatment of TMJ using MET has been limited in its documentation, although MET may have beneficial outcome on the pain frequently seen in TMD. MET is useful in reducing tension in the jaw muscle, improving joint motion and subsequently reducing pain, be it localized or referred to the face and head. MET is of considerable value in the resolution of the musculoskeletal component of TMJ pain and dysfunction (Royder, 1981). As MET works on both the TMJ and the muscles of mastication (mainly the temporalis and masseter) it is considered to be appropriate for treating both the limitation of mouth opening and the muscular component (strain and/or hypertonicity) of TMD (Chiatow, 2006).
MATERIALS AND METHODS
The study was approved by the Human Ethics and Institutional Review Committee of Vikas College of Physiotherapy, Mangalore. This research project was conducted from June 2008 to May 2009. The participants included in this study included adults aged 20-30 years of both sexes, who were diagnosed by Dentists, as having unilateral TMD based on clinical findings and imaging techniques.
| Table 1: | Exclusion and inclusion criteria |
 | |
Initially, simple random sampling identified 50 participants, each receiving a self-report questionnaire by mail. Of the 50 targeted, 40 participants returned the survey; a response rate of 80%. Participants completed demographic questions such as age, gender and marital status as well as information specific to the level of impairment of their report of TMJ pain. All participants were asked about the frequency of their TMJ pain. They were evaluated by physical examination, viz., observation, palpation, pain assessment and joint range of motion (inter-incisal distance) assessment. The participants, who fulfilled the inclusion and exclusion criteria (Table 1), were explained about the purpose of the study, types of evaluation and intervention procedures to undergo as part of the study. Assurance was given that their identity will be concealed, but informed that the results of the study will be disseminated among other professionals and even may be published in professional journals. The subjects were then encouraged to ask any questions and clarifications regarding the purpose of the study and their anxieties and doubts were cleared. A written informed consent was obtained. Participants were treated with MET which includes post isometric relaxation and reciprocal inhibition, thrice a week for 5 weeks. The duration of each contraction was 10 sec and was repeated for 5 times.
Evaluation was carried out for the level of self-reported pain and TMJ range of motion, in case of each subject, before the commencement of interventions and at the end of each week of interventions. Pain was measured using Visual Analogue Scale, which is a 10 cm horizontal line. The left end of the line was marked 0 which represents no pain at all and the right end of the line was marked 10, which represents the worst pain imaginable by the subject. The subjects were told to mark the intensity of the pain perceived on the scale. The TMJ range of motion was measured as the Maximum Mouth Opening (MMO) and measurement was taken with a transparent plastic ruler as the participant actively opened his/her mouth to the maximum possible distance. The distance between the upper central incisors and the lower central incisors was determined as the inter-incisor range of opening (Harrison, 1997).
Statistical analysis: The collected data were analyzed using the statistical tests. The data collected by MMO were analyzed using parametric tests as the data is interval in nature. The intra group pre and post-test data for MMO were analyzed using paired t-test, while the post-test inter group data were analyzed with unrelated t-test. The data collected by visual analog scale were analyzed using non-parametric tests as the data is ordinal in nature. The intra group pre and post-test VAS scores was analyzed using Wilcoxon signed rank test and post-test inter group VAS scores were analyzed with Mannwhitney U-test. The statistical significance of the p-value for all the analyzed data was fixed at 0.05.
RESULTS
The study consisted of 40 participants (n = 40), with a gender distribution of 21 females (55%) and 19 males (45%). The age of the participants ranged between 20 and 30 and the mean was 25.5±2.96. The mean duration of symptoms for the participants was 47.7±23.85 days. Within same group, the comparison of pain as measured by VAS at the end of each week of intervention. Results are presented in Table 2 and 3. It clearly shows that there was a gradual and definitive reduction in the self reported pain on a week-on-week basis as reflected in the median values.
The median score for the pre-test by VAS was 7, which reduced to 6 at the end of week 1, 5 at the end of week 2, 4 at the end of week 3, 3 at the end of week 4 and 1 at the end of the 5 week intervention period. Further the results showed that when compared with the pre-test VAS value, the reduction in level of pain at the end of each week and at the end of the 5 week intervention period is statistically significant (p<0.05) (Table 3).
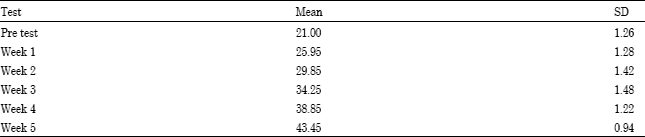
Similarly, the MMO scores show that there is considerable increase between the pre test value and post test value. Moreover the MMO scores recorded at the end of each week of intervention also shows gradual improvement. The pre test mean MMO score was 21±1.26. At the end of week 1, the mean MMO scores showed a remarkable improvement with the value of 25.95±1.28 (Table 4). This improvement was maintained in subsequent weeks as can be seen from the values measured at the end of each week.
It shows that the Mean Difference (MD) between the pre test sore and the score at the end of week 1 is 4.95. The statistical analysis (t-value = 56.18) reveals that the improvement in MMO value is statistically significant (p-value = 0.00). The improvement in MMO value at the end of week 2 when compared to the pre test value showed a MD of 8.85, which was statistically significant (t-value = 67.41, p-value = 0.00). At the end of week 3 the MMO scores showed a MD of 13.25 when compared to the pre test value, which on statistical analysis (t-value =85.08) showed a significant improvement (p-value = 0.000). The MD in MMO at the end of week 4 when compared to the baseline was 17.85 and on analysis (t-value = 107.13) it showed a significant improvement (p-value = 0.000).
| Table 2: | Pre test and week wise VAS score |
 | |
| Table 3: | Pre-post test comparison of VAS score |
 | |
| *p<0.05 is statistically significant | |
| Table 4: | Pre test and week wise mean and Standard Deviation (SD) of MMO |
 | |
| Table 5: | Pre-Post test comparison of MMO |
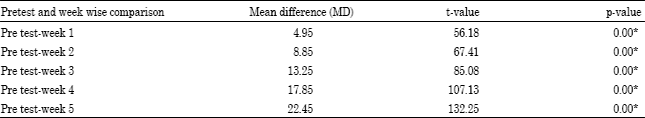 | |
| *p<0.05 is statistically significant | |
The post test MMO score at the end of the 5 week intervention period when compared to the pre test score showed a MD of 22.45, which on statistical analysis (t-value = 132.25) revealed a significant improvement (p-value =0.000) (Table 5).
DISCUSSION
MET reduces tension in the jaw muscles and subsequently reduces pain, be it localized or referred to the face and head (Royder, 1981). In the present study MMO increased, it is similar to the findings by Anderson (Anderson, 2004). The MET stimulates the muscle spindles and Golgi tendon organs reducing excessive activity (Bell, 1990). Stretching of the muscle fibers stimulates the Golgi tendon receptors, which have an inhibitory influence on muscle tension, leading to muscle relaxation (Roberts, 1997). When a muscle is actively contracted, its antagonists are reflexively relaxed (Royder, 1981). Therefore, opening the mouth against resistance is inclined to relax contracted elevator muscle and vice versa for opening muscles (Royder, 1981), which can increase the ROM. However findings of present study did not support the work of Gosling and Frois (2004) and Freshwater and Gosling (2003). The reduction in pain by MET is similar to the findings by Lewit and Simons (1984) and Brodin (1982). Although, Brodin’s work was involved with the treatment of lumbar spine rather than TMJ, it is reasonable to assume that the mechanisms involved are similar. The possible reason for this discrepancy is that both the studies involved only a single session of MET which may not have been adequate in bringing about positive results.
Limitations of the study:
| • | The study duration was short, only 5 weeks and the results apply to short term only, which might differ in the longer run |
| • | No long term follow up was done to ascertain the differences in long term gains in the protocols |
| • | Sample size taken for the study is small and bigger sample might have led to some differences in the results |
| • | Limited parameter of outcome measure was used which might bias the results |
This study showed that, muscle energy technique demonstrated a significant reduction in TMJ pain and increase in TMJ range of motion as measured by Maximal mouth opening after five weeks of intervention in TMD. However, due to the lack of control group, small sample size and a dearth in the literature supporting the findings of this study, the results should be interpreted with caution.
REFERENCES
- De Wijer, A., J.R. de Leeuw, M.H. Steenks and F. Bosman, 1996. Temporomandibular and cervical spine disorders: Self-reported signs and symptoms. Spine, 21: 1638-1646.
Direct Link - Di Fabio, R.P., 1998. Physical therapy for patients with TMD: A descriptive study of treatment, disability and health status. J. Orofacial Pain, 12: 124-135.
PubMed - Goulet, J.P., G.J. Lavigne and J.P. Lund, 1995. Jaw pain prevalence among French-speaking Canadians in Quebec and related symptoms of temporomandibular disorders. J. Dental Res., 74: 1738-1744.
PubMed - Gremillion, H.A., 2000. The prevalence and etiology of tempormandibular disorders and orofacial pain. Texes Dental J., 117: 30-39.
PubMed - Griffiths, R.H., 1983. Report of the President`s conference on examination, diagnosis and management of temporomandibular disorders. Am. J. Orthodontics, 83: 514-517.
CrossRef - Lewit, K. and D.G. Simons, 1984. Myofacial pain: Relief by post-isometric relaxation. Arch. Phys. Med. Rehabilitation, 65: 452-456.
PubMed - Morris, S., S. Benjamin, R. Gray and D. Bennet, 1997. Physical, psychiatric and social characteristics of the temperomandibular disorder pain dysfunction syndrome: The relationship of mental disorders to presentation. Br. Dental J., 182: 255-260.
PubMed - Roberts, B.L., 1997. Soft tissue manipulation: Neuromuscular and muscle energy technique. J. Neurosci. Nursing, 29: 123-127.
PubMed - Rocabado, M., 1987. The importance of soft tissue mechanics in stability and instability of the cervical spine: A functional diagnosis for treatment planning. Cranio, 5: 130-138.
PubMed - Royder, J.O., 1981. Structural influences in temporomandibular joint pain and dysfunction. J. Am. Osteopathic Assoc., 80: 460-467.
PubMed - Rugh, J.D. and W.K. Solberg, 1985. Oral health status in United States: Temporomandibular disoreders. J. Dental Educ., 49: 398-406.
PubMed - Saghafi, D. and D. Curl, 1995. Chiropractic manipulation of anteriorly displaced temporomandibular disc with adhesion. J. Manipulative Physiol. Ther., 18: 98-104.
PubMed - Yap, A.U., E.K. Chua and J.K. Hoe, 2002. Clinical TMD, pain-related disability and psychological status of TMD patients. J. Oral Rehabil., 29: 374-380.
Direct Link - Yap, A.U.J. and V.C.L. Ho, 1999. Temporomandibular disorders-an overview. Singapore Med. J., 40: 179-182.
Direct Link








