Research Article
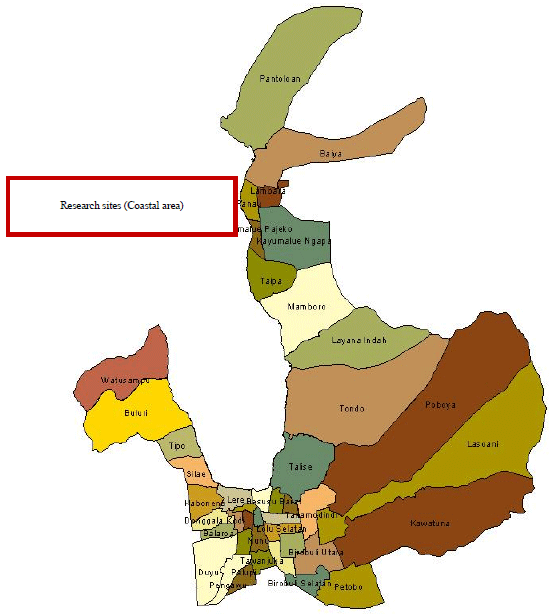
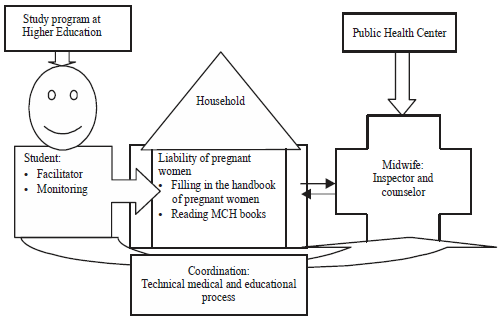
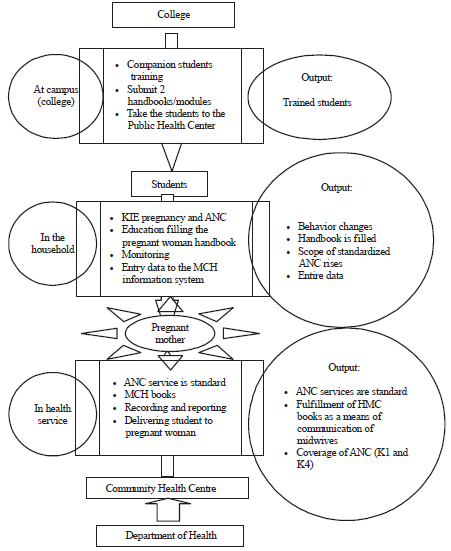
Household-based Antenatal Care Monitoring Model (An Intervention Study in the Coastal Area of Palu City)
Department of Public Health Science, Faculty of Medicine, Tadulako University, Palu, Indonesia
Muh. Syafar
Health Education and Promotion, Faculty of Public Health, Hasanuddin University, Makassar, Indonesia
Nurhaedar Jafar
Nutritional Study Program, Faculty of Public Health, Hasanuddin University, Makassar, Indonesia
Masni
Department of Biostatistics, Faculty of Public Health, Hasanuddin University, Makassar, Indonesia
Anwar Mallongi
Department of Environmental Health, Faculty of Public Health, Hasanuddin University, Makassar, Indonesia
LiveDNA: 62.16355