Research Article
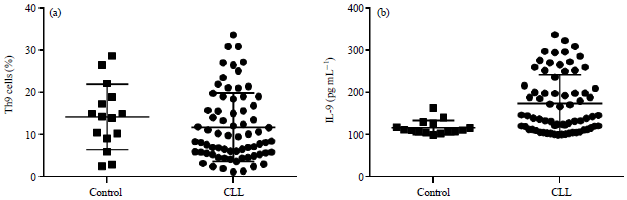
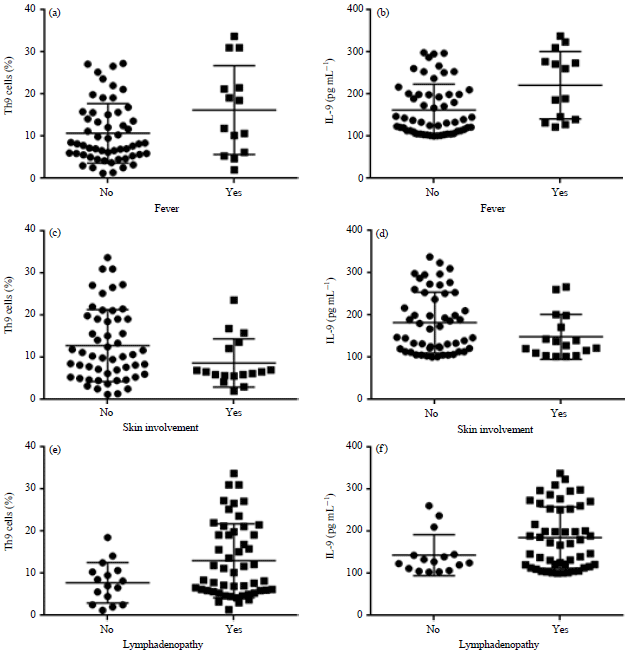
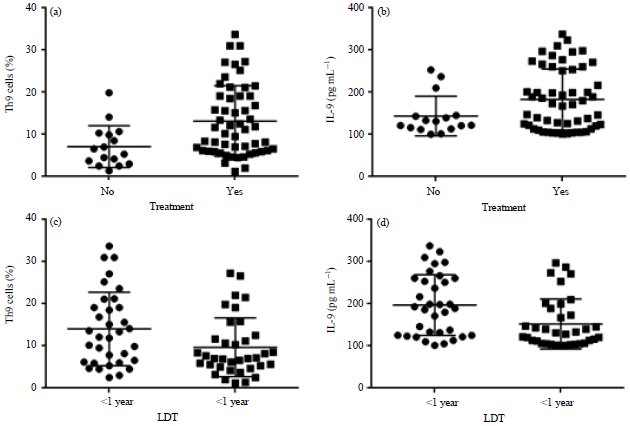
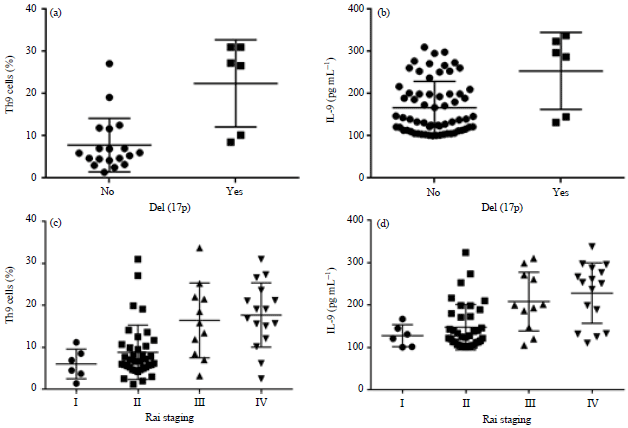
Prognostic Role of T Helper 9 Cells and Interleukin-9 in Chronic Lymphocytic Leukemia
Division of Biochemistry, Department of Chemistry, Faculty of Science, Mansoura University, 35516, Mansoura, Egypt
Fardous F. El-Senduny,
Division of Biochemistry, Department of Chemistry, Faculty of Science, Mansoura University, 35516, Mansoura, Egypt
Nashwa K. Abousamra
Department of Clinical Pathology, Hematology Unit, Faculty of Medicine, Mansoura University, 35516, Mansoura, Egypt
Manal Salah EL-Din
Department of Medical Oncology, Oncology Center, Mansoura University, 35516, Mansoura, Egypt
Magdy M. Youssef
Division of Biochemistry, Department of Chemistry, Faculty of Science, Mansoura University, 35516, Mansoura, Egypt
LiveDNA: 20.3339