ABSTRACT
Keeping in mind the difficulty faced by patients during continuous use of the mold, after vaginal reconstruction a novel mold and harness was designed to increase patient compliance. Reported here are three cases of transverse vaginal septum where presenting complaint was primary infertility. Postoperative mold use and follow up is crucial to prevent restenosis and achieve optimum success after vaginal reconstruction. This novel mold and harness system increased patient compliance and thus was helpful in achieving successful outcome.
PDF Abstract XML References Citation
How to cite this article
DOI: 10.3923/rjog.2011.59.63
URL: https://scialert.net/abstract/?doi=rjog.2011.59.63
INTRODUCTION
Transverse vaginal septum is a vertical fusion defect as classified in American Society of Reproductive Medicine (ASRM) classification of uterovaginal anomalies (Anonymous, 1988).
The most worrying aspect of vaginal reconstruction is the risk of post-operative stenosis. In order to prevent this complication strict compliance to the use of vaginal mold during the constrictive phase of healing is a required. However, unlike vaginoplasty, scant information is provided in literature concerning molds used after resection of vaginal septa (Lacy et al., 2007). We present here three cases of transverse vaginal septum where presenting complaint was primary infertility. Keeping in mind the difficulty faced by patients during continuous use of the mold, a novel mold and harness was designed with the help of an occupational therapist to increase patient compliance.
MATERIALS AND METHODS
Patient 1: Presented in August 2007 at the age of 33 years with primary infertility for ten years. Her menstrual cycles had always been regular with mild spasmodic dysmenorrhea. She never had coital difficulties. While undergoing infertility work up in a private hospital, she was detected to have a transverse vaginal septum five years ago, for which septal resection was done. She was not advised to use vaginal mold postoperatively. Ovulation induction with intrauterine insemination was tried with no success.
On speculum examination, blind vagina measuring 5 cm was noted. Cervix was not visualized. A high transverse vaginal septum was present with a small sinus opening. On bimanual rectal examination cervix was felt. Transvaginal Sonography (TVS) revealed uterus with three small fibroids. Both the ovaries had endometriotic cyst (right: 4, left: 2.4 cm). Husband’s semen analysis was within normal limits. Laparotomy with bilateral ovarian cystectomy and transverse vaginal septum resection was performed. A vaginal mold made of thermoplastic material was inserted for one week. She was advised to use a new mold made of dental material for six weeks and to remove it only during urination and defecation. Later for another six weeks she used the mold only during nights. No vaginal constriction was evident at three months, after reconstruction.
Patient 2: Presented in May 2008, at the age of 30 with primary infertility. She was married for four years. Her menstrual cycles were regular with mild dysmenorrhea. She had received two cycles of ovulation induction with clomiphene citrate 50 mg, follicular imaging and timed intercourse two years ago. On speculum examination a transverse vaginal septum was noted with a small opening at 3 O’ clock position. TVS confirmed a high vaginal septum 6-8 mm thick, with minimal collection above it. After complete resection of the septum, upper end of the vagina was anastomosed with its lower end. Vaginal mold made of thermoplastic material was placed in situ and sutured to the labia. Mold was changed on sixth post operative day. She was advised to use it continuously for six weeks and to remove it only during urination and defecation. After one month of usage, patient complained of itching and redness in and around her vagina. Thermoplastic mold was then changed to mold made of dental material and was advised to use it only during night. After two weeks patient discontinued using the mold on her own. No vaginal constriction was evident during vaginal examination, two months postoperatively. Patient was advised regular intercourse. One year later she conceived spontaneously. Antenatal period was uneventful. She underwent elective cesarean delivery in view of Cephalopelvic Disproportion (CPD) and delivered a male baby weighing 4180.
Patient 3: Presented in August 2008 at the age of 28 years with primary infertility of one and a half year duration and was referred for vaginal atresia. She complained of dyspareunia. She had dysmenorrhea during regular menstrual cycles. On speculum examination she had blind vagina which was 2 cm in length with a sinus like hole through which menstrual blood was draining. Diagnosis of a low transverse vaginal septum was made. TVS showed normal uterus and ovaries, though cervix could not be clearly visualized. To rule out cervical agenesis Magnetic Resonance Imaging (MRI) was done. MRI revealed minimal fluid within endometrial and endocervical cavity. Proximal vaginal cavity and vaginal fornices were also visualized. Intraoperatively low transverse vaginal septum was noted with a small sinus. Blunt dissection of loose areoalar tissue was done. Thick band of upper part of vaginal septum was excised, followed by end to end anastomosis of upper and lower vaginal flaps. Thermoplastic mold was placed in situ which was sutured with labia. Thermoplastic mold was changed on sixth postoperative day to mold made of dental material. She used it continuously with the harness for next six weeks, removing only during micturition and defecation. Later she used the mold only during nights for the next six weeks. Postoperative compliance with dilatation was good and no vaginal constriction was evident at three months after vaginal reconstruction.
RESULTS AND DISCUSSION
All three patients reported here presented with primary infertility, transverse vaginal septum and regular menstrual cycles. In patient 2 the finding of vaginal septum was completely missed.
Patient 1 though had history of vaginal septum resection, either it was an incomplete resection of the septum or restenosis due to failure to use vaginal mold postoperatively. The main long-term complication of septum resection is vaginal stenosis which may be treated with dilation or require further surgery. To prevent stenosis, it is recommended that postoperatively the patient wears a mold continuously for the subsequent two months. After this, she should continue to wear the stent at nighttime during the following four months of the healing phase (Quint et al., 2010). In present experience mold use for three months gave us comparable results.
Ideally, the mold should be inexpensive, easy to make, comfortable to wear, should allow drainage of physiological uterocervical discharge and vaginal discharge during healing phase. To fulfill all these prerequisites a low temperature thermoplastic (aquaplast material, coated, 2.1 mm thickness for non-perforated mold and 3.1 mm thickness for perforated mold) mold was designed. The molds are hollow cylinders with both ends open. Initial molds were nonperforated with greater rigidity. Presently molds are being made of perforated plastic for better wound drainage during healing phase (Fig. 1). The mold has three parts: (1) a molded tip (2) hollow cylindrical body and (3) a base. Diameter of the cylindrical body is 2.5 cm and its length varies from 5 to 10 cm, depending upon the site of septum (high, mid or low). The base has been contoured to adjust well with the pubic contour.
With our prior experience with vaginoplasties, we realized that wearing of mold without a support is a practical problem. Thus, for all these patients a harness was designed to hold the mold in place. The harness (Fig. 2) has a waist strap and two (anterior and postetrior) perineal straps. Waist strap is made of 2 wide cotton tape with 2 Stainless Steel (SS) D-ring and velcro. Anterior and posterior perineal straps are made of 1 wide cotton tape with anterior strap 1.5 longer than the posterior one. These perineal straps join the waist strap with the help of a velcro. On the other side these perineal straps are attached to the outer surface of base of the mold by inserting these into a slot created for this purpose. Tightening of the harnessing system is as per the comfort of patient and stability of the splint.
For the first case the harnessing system comprised of four perineal straps-two anterior and two posterior, all crossing over at the base of the mold, in order to provide angular stability (Fig. 3). In the latest design method of attachment has been upgraded, making it possible to produce similar stability by using two straps, thus debulking the harnessing system.
Contrary to the available literature (Lacy et al., 2007) where elastic belt has been used, we used cotton which is a natural fabric and complies well with skin. It is flat and has some amount of natural rigidity, thus is mechanically more stable.
 | |
| Fig. 1: | Termoplastic vaginal mold (perforated): (1) Molded tip (2) Cylindrical body (3) Flared base |
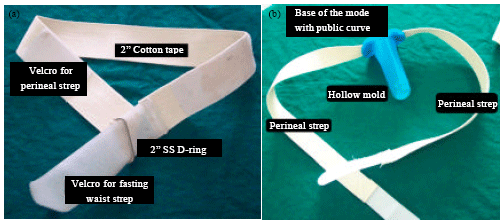 | |
| Fig. 2(a-b): | Latest harness design, having (a) waist strap and (b) only two perineal straps (anterior and posterior |
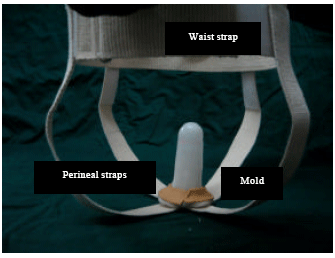 | |
| Fig. 3: | Earlier harness with mold in place, having waist strap and four perineal straps |
Present approach is very cost effective with total cost of the splint being INR 525 (equivalent to USD 12, Euro 8). Making time is 30 to 45 min. In our institute the department of occupational therapy has also developed a kit for easy designing and fabrication of the splint which substantially reduces the mold making time. It also facilitates making molds with different specifications.
For all our patients this harness made continuous wearing of the mold much easier and definitely increased patient’s compliance. Once the vagina is healed well in sexually active women regular intercourse is sufficient to maintain its patency.
Patient 1 at the time of presentation had already developed chocolate cysts in both the ovaries. This case demonstrates how delay in diagnosis and inappropriate management of transverse vaginal septum can lead to retrograde menstruation and endometriosis, adding onto the problem with fertility.
It is imperative to differentiate cases of high transverse vaginal septum from cervical dysgenesis before planning surgical management. As complications of recanalizing the cervix are common and the possibility of a viable pregnancy is unlikely (Rock et al., 1984; Hampton, 1990) MRI as shown in case 3 is an important diagnostic tool to rule out cervical agenesis in case of doubt (Lopez et al., 2005).
Transverse vaginal septum also presents surgical challenges. A thin septum can be repaired relatively easily with an end-to-end anastamosis (Miller and Breech, 2008). Thicker septa, however, may require undermining the vaginal mucosa to allow the lower vagina to reach the upper vagina. To decrease the risk of postoperative stenosis, a Z-plasty may be performed (Wierrani et al., 2003). If the septum is very thick, a skin graft may be required to reanastamose the lower and upper vagina. Conversely, when a young girl presents with acute symptoms due to collection of blood in cases of transverse vaginal septum, surgical drainage is the treatment of choice. A novel technique of laparoscopic drainage to relieve acute symptoms has been described recently (Dennie et al., 2010). In all three cases of our series irrespective of its thickness septal resection and end to end anastomosis of vaginal walls coupled with postoperative mold usage followed by regular sexual activity provided satisfactory results.
CONCLUSION
Postoperative mold use and follow up is important to prevent restenosis and achieve optimum success after vaginal reconstruction. This can be facilitated by thorough counseling and incorporation of a harness to hold the mold in place. Both the mold and the harness are inexpensive and easily replicable. Thus properly guided postoperative use of vaginal mold with a harness may decrease the need of reoperations.
REFERENCES
- Anonymous, 1988. The American fertility society classifications of adnexal adhesions, distal tubal occlusion, tubal occlusion secondary to tubal ligation, tubal pregnancies, mullerian anomalies and intrauterine adhesions. Fertil. Steril., 49: 944-955.
PubMed - Quint, E.H., J.D. McCarthy and Y.R. Smith, 2010. Vaginal surgery for congenital anomalies. Clin. Obstet. Gynecol., 53: 115-124.
PubMed - Lacy, J., G.R. Correll, D.K. Walmer and T.M. Price, 2007. Simple vaginal mold for use in the postoperative care of patients with a transverse vaginal septum. Fertil. Steril., 87: 1225-1226.
PubMed - Rock, J.A., W.D. Schlaff, H.A. Zacur and H.W. Jones Jr., 1984. The clinical management of congenital absence of the uterine cervix. Int. J. Gynaecol. Obstet., 22: 231-235.
PubMed - Hampton, H.L., 1990. Role of the gynecologic surgeon in the management of urogenital anomalies in adolescents. Curr. Opin. Obstet. Gynecol., 2: 812-818.
PubMed - Lopez, C., M. Balogun, R. Ganesan, J.F. Olliff, 2005. MRI of vaginal conditions. Clin. Radiol., 60: 648-662.
PubMed - Miller, R. and L. Breech, 2008. Surgical correction of vaginal anomalies. Clin. Obstet. Gynecol., 51: 223-236.
PubMed - Wierrani, F., K. Bodner, B. Spangler and W. Grunberger, 2003. Z-Plasty of the transverse vaginal septum using Garcia's procedure and the Grunberger modification. Fertil. Steril., 79: 608-612.
CrossRef - Dennie, J., S. Pillay, D. Watson and S. Grover, 2010. Laparoscopic drainage of hematocolpos: A new treatment option for the acute management of a transverse vaginal septum. Fertil. Steril., 9: 1853-1857.
PubMed








