Research Article
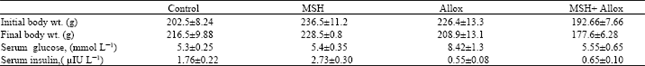
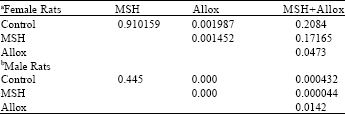
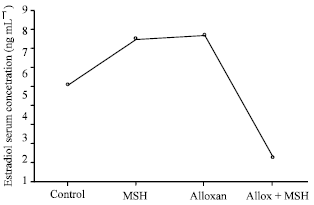
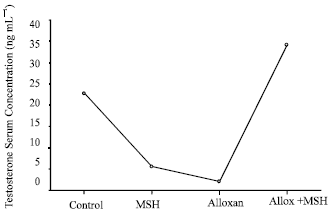
Effects of Melanocyte-stimulating Hormone on Plasma Levels of Testosterone and Estradiol Hormones in Alloxan-Induced Diabetic Rats
Department of Medical Technology, Faculty of Allied Medical Sciences, Applied Science University, Amman, Jordan
Fahmi Mahmoud
Faculty of Pharmacy, Al-Zaytoonah University of Jordan, Amman Jordan
Moayad Khataibeh
Department of Medical Technology, Faculty of Allied Medical Sciences, Applied Science University, Amman, Jordan
Suhail Hamdan
Medical School, Al-Quds University, Al-Quds, Palestine
Aurelia Crevoi
Department of Human and Animal Physiology, Moldova State University, Moldova